Orgasmic dysfunction
Inhibited sexual excitement; Sex - orgasmic dysfunction; Anorgasmia; Sexual dysfunction - orgasmic; Sexual problem - orgasmic
Orgasmic dysfunction is when a woman either cannot reach orgasm, or has trouble reaching orgasm when she is sexually excited.
When sex is not enjoyable, it can become a chore instead of a satisfying, intimate experience for both partners. Sexual desire will often decline, and sex occurs less often. This can create resentment and conflict in the relationship.
Causes
About 10% to 15% of women have never had an orgasm. Surveys suggest that up to one half of women are not satisfied with how often they reach orgasm.
Sexual response involves the mind and body working together in a complex way. Both need to function well for an orgasm to happen.
Many factors can lead to problems reaching orgasm. They include:
- A history of sexual abuse or rape
- Boredom in sexual activity or a relationship
-
Fatigue and
stress
or
depression
Stress
Stress is a feeling of emotional or physical tension. It can come from any event or thought that makes you feel frustrated, angry, or nervous. Stres...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark ArticleDepression
Depression may be described as feeling sad, blue, unhappy, miserable, or down in the dumps. Most of us feel this way at one time or another for shor...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Lack of knowledge about sexual function
- Negative feelings about sex (often learned in childhood or teen years)
- Shyness or embarrassment about asking for the type of touching off that works best
Health problems that can cause problems reaching orgasm include:
- Certain drugs that are prescribed. The most common drugs used to treat depression may cause this problem. These include fluoxetine (Prozac), paroxetine (Paxil), and sertraline (Zoloft)
- Hormonal disorders or changes, such as menopause
- Chronic illnesses that affect health and sexual interest
- Chronic pelvic pain, such as from endometriosis
- Damage to the nerves that supply the pelvis due to conditions such as multiple sclerosis, diabetic nerve damage, and spinal cord injury
-
Spasm of the muscles surrounding the vagina
that occurs against your will
Spasm of the muscles surrounding the va...
Vaginismus is a spasm of the muscles surrounding the vagina that occurs against your will. The spasms close the vagina and can prevent sexual activi...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Vaginal dryness
Vaginal dryness
Vaginal dryness is present when the tissues of the vagina are no longer well-lubricated and healthy.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
Symptoms
The symptoms of orgasmic dysfunction include:
- Being unable to reach orgasm
- Taking longer than you want to reach orgasm
- Having only unsatisfying orgasms
Exams and Tests
A complete medical history and physical exam needs to be done, but results are almost always normal. If the problem began after starting a medicine, tell the health care provider who prescribed the drug. A qualified specialist in sex therapy may be helpful.
Treatment
Important goals when treating problems with orgasms are:
- A healthy attitude toward sex, and education about sexual stimulation and response
- Learning to clearly communicate sexual needs and desires, verbally or non-verbally
How to make sex better:
- Get plenty of rest and eat well. Limit alcohol, drugs, and smoking. Feel your best. This helps with feeling better about sex.
- Do Kegel exercises. Tighten and relax the pelvic muscles.
- Focus on other sexual activities, not just intercourse.
- Use birth control that works for both you and your partner. Discuss this ahead of time so you aren't worried about an unwanted pregnancy.
- If other sexual problems, such as lack of interest and pain during intercourse, are happening at the same time, these need to be addressed as part of the treatment plan.
Discuss the following with your provider:
- Medical problems, such as diabetes or multiple sclerosis
- New medicines
- Menopausal symptoms
The role of taking female hormone supplements in treating orgasmic dysfunction is unproven and the long-term risks remain unclear.
Treatment can involve education and learning to reach orgasm by focusing on pleasurable stimulation, and directed masturbation.
- Most women require clitoral stimulation to reach an orgasm. Including clitoral stimulation in sexual activity may be all that is necessary.
- If this does not solve the problem, then teaching the woman to masturbate may help her understand what she needs to become sexually excited.
Treatment may include sexual counseling to learn series of couples' exercises to:
- Learn and practice communication
- Learn more effective stimulation and playfulness
Outlook (Prognosis)
Women do better when treatment involves learning sexual techniques or a method called desensitization. This treatment gradually works to decrease the response that causes lack of orgasms. Desensitization is helpful for women with significant sexual anxiety.
References
Biggs WS, Chaganaboyana S. Human sexuality. In: Rakel RE, Rakel DP, eds. Textbook of Family Medicine . 9th ed. Philadelphia, PA: Elsevier; 2016:chap 42.
Cowley DS, Lentz GM. Emotional aspects of gynecology: depression, anxiety, post-traumatic stress disorder, eating disorders, substance abuse, "difficult" patients, sexual function, rape, intimate partner violence, and grief. In: Lobo RA, Gershenson DM, Lentz GM, Valea FA, eds. Comprehensive Gynecology . 7th ed. Philadelphia, PA: Elsevier; 2017:chap 9.
-
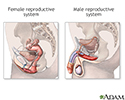
Male and female reproductive systems - illustration
The male and female reproductive systems, viewed from a mid-sagittal section.
Male and female reproductive systems
illustration
Review Date: 5/16/2016
Reviewed By: Irina Burd, MD, PhD, Associate Professor of Gynecology and Obstetrics at Johns Hopkins University School of Medicine, Baltimore, MD. Review provided by VeriMed Healthcare Network. Also reviewed by David Zieve, MD, MHA, Isla Ogilvie, PhD, and the A.D.A.M. Editorial team.