Head and face reconstruction
Craniofacial reconstruction; Orbital-craniofacial surgery; Facial reconstruction
Head and face reconstruction is surgery to repair or reshape deformities of the head and face (craniofacial).
Description
How surgery for head and face deformities (craniofacial reconstruction) is done depends on the type and severity of deformity, and the person's condition.
Surgical repairs involve the skull (cranium), brain, nerves, eyes, facial bones, and facial skin. That is why sometimes a plastic surgeon (for skin and face) and a neurosurgeon (brain and nerves) work together. Head and neck surgeons also perform craniofacial reconstruction operations.
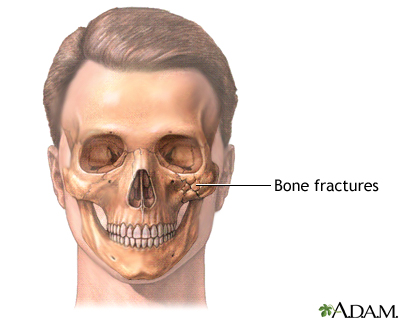
The surgery is done while you are deep asleep and pain-free (under general anesthesia ). The surgery may take 4 to 12 hours or more. Some of the bones of the face are cut and moved. During the surgery, tissues are moved and blood vessels and nerves are reconnected using microscopic surgery techniques.
General anesthesia
General anesthesia is treatment with certain medicines that puts you into a deep sleep so you do not feel pain during surgery. After you receive the...
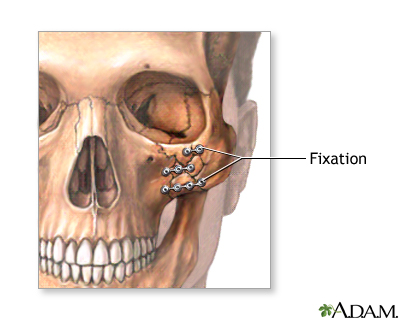
Pieces of bone ( bone grafts ) may be taken from the pelvis, ribs, or skull to fill in spaces where bones of the face and head were moved. Small metal screws and plates may be used to hold the bones in place. The jaws may be wired together to hold the new bone positions in place. To cover the holes, flaps may be taken from the hand, buttocks, chest wall, or thigh.
Bone grafts
A bone graft is surgery to place new bone or bone substitutes into spaces around a broken bone or bone defects.
Sometimes the surgery causes swelling of the face , mouth, or neck, which may last for weeks. This can block the airway. For this, you will need to have a temporary tracheotomy. This is a small hole that is made in your neck through which a tube (endotracheal tube) is placed in the airway (trachea). This allows you to breathe when your face and upper airway are swollen.
Swelling of the face
Facial swelling is the buildup of fluid in the tissues of the face. Swelling may also affect the neck and upper arms.

Why the Procedure is Performed
Craniofacial reconstruction may be done if there are:
-
Birth defects and deformities from conditions such as
cleft lip or palate
,
craniosynostosis
,
Apert syndrome
Cleft lip or palate
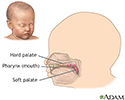
Cleft lip and palate are birth defects that affect the upper lip and the roof of the mouth.
 ImageRead Article Now Book Mark Article
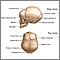
ImageRead Article Now Book Mark ArticleCraniosynostosis
Craniosynostosis is a birth defect in which one or more of the sutures on a baby's head closes earlier than usual. The skull of an infant or young c...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark ArticleApert syndrome
Apert syndrome is a genetic disease in which the seams between the skull bones close earlier than normal. This affects the shape of the head and fac...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Deformities caused by surgery done to treat tumors
- Injuries to the head, face, or jaw
- Tumors
Risks
Risks of anesthesia and surgery in general are:
- Problems breathing
- Reactions to medicines
- Bleeding, blood clots, infection
Risks of surgery of the head and face are:
- Nerve (cranial nerve dysfunction) or brain damage
- Need for follow-up surgery, especially in growing children
-
Partial or total loss of
bone grafts
Bone grafts
A bone graft is surgery to place new bone or bone substitutes into spaces around a broken bone or bone defects.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Permanent scarring
These complications are more common in people who:
- Smoke
- Have poor nutrition
-
Have other medical conditions, such as
lupus
Lupus
Systemic lupus erythematosus (SLE) is an autoimmune disease. In this disease, the body's immune system mistakenly attacks healthy tissue. It can af...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Have poor blood circulation
- Have past nerve damage
After the Procedure
You may spend the first 2 days after surgery in the intensive care unit. If you do not have a complication, you will be able to leave the hospital within 1 week. Complete healing may take 6 weeks or more.
Outlook (Prognosis)
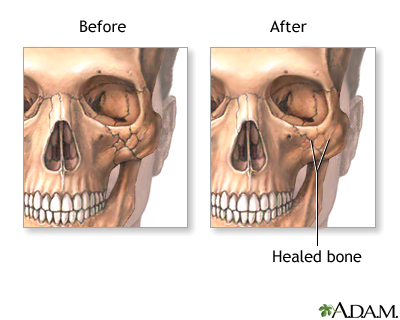
A much more normal appearance can be expected after surgery. Some people need to have follow-up procedures during the next 1 to 4 years.
It is important not to participate in contact sports for 2 to 6 months after surgery.
People who have had a serious injury often need to work through the emotional issues of the trauma and the change in their appearance. Children and adults who have had a serious injury may have post-traumatic stress disorder, depression, and anxiety disorders. Talking to a mental health professional or joining a support group can be helpful.
Parents of children with deformities of the face often feel guilty or ashamed, especially when the deformities are due to a genetic condition. As younger children grow and become aware of their appearance, emotional symptoms may develop or get worse.
References
Baker SR. Reconstruction of facial defects. In: Flint PW, Haughey BH, Lund V, et al., eds. Cummings Otolaryngology: Head & Neck Surgery . 6th ed. Philadelphia, PA: Elsevier Mosby; 2015:chap 24.
McGrath MH, Pomerantz J. Plastic surgery. In: Townsend CM, Beauchamp RD, Evers BM, Mattox KL, eds. Sabiston Textbook of Surgery . 19th ed. Philadelphia, PA: Elsevier Saunders; 2012:chap 69.
-
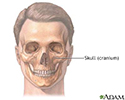
Skull - illustration
The skull is anterior to the spinal column and is the bony structure that encases the brain. Its purpose is to protect the brain and allow attachments for the facial muscles. The two regions of the skull are the cranial and facial region. The cranial portion is the part of the skull that directly houses the brain and the facial portion includes the rest of the bones of the skull.
Skull
illustration
-
Skull - illustration
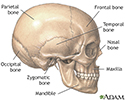
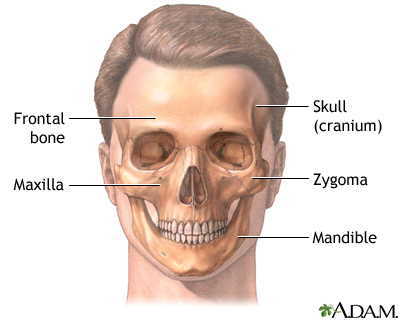
The skull is the bony structure of the head and face. The cranium surrounds the brain with the temporal, frontal, parietal and occipital bones. The maxilla, or upper jaw, and the mandible, or lower jaw, support the facial features of nose, mouth and eyes.
Skull
illustration
-
Cleft lip repair - series
Presentation
-
Craniofacial reconstruction - series
Presentation
-
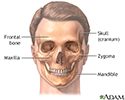
Skull - illustration
The skull is anterior to the spinal column and is the bony structure that encases the brain. Its purpose is to protect the brain and allow attachments for the facial muscles. The two regions of the skull are the cranial and facial region. The cranial portion is the part of the skull that directly houses the brain and the facial portion includes the rest of the bones of the skull.
Skull
illustration
-
Skull - illustration
The skull is the bony structure of the head and face. The cranium surrounds the brain with the temporal, frontal, parietal and occipital bones. The maxilla, or upper jaw, and the mandible, or lower jaw, support the facial features of nose, mouth and eyes.
Skull
illustration
-
Cleft lip repair - series
Presentation
-
Craniofacial reconstruction - series
Presentation
Review Date: 4/14/2015
Reviewed By: Hebe Molmenti, MD, PhD, private practice specializing in plastic and reconstructive surgery, Baltimore, MD. Review provided by VeriMed Healthcare Network. Also reviewed by David Zieve, MD, MHA, Isla Ogilvie, PhD, and the A.D.A.M. Editorial team.