Stroke
Cerebrovascular disease; CVA; Cerebral infarction; Cerebral hemorrhage; Ischemic stroke; Stroke - ischemic; Cerebrovascular accident; Stroke - hemorrhagic; Carotid artery - stroke
A stroke occurs when blood flow to a part of the brain stops. A stroke is sometimes called a "brain attack."
If blood flow is cut off for longer than a few seconds, the brain cannot get nutrients and oxygen. Brain cells can die, causing lasting damage.
Causes
There are two major types of stroke:
- Ischemic stroke
- Hemorrhagic stroke
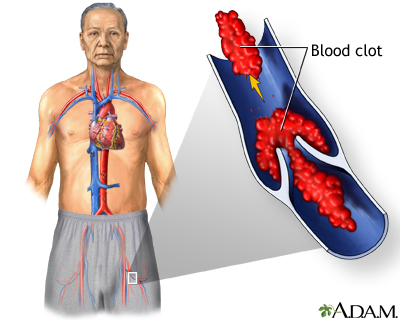
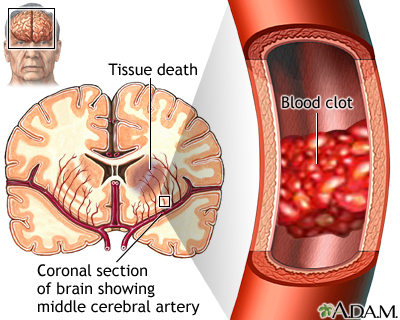
Ischemic stroke occurs when a blood vessel that supplies blood to the brain is blocked by a blood clot. This may happen in two ways:
- A clot may form in an artery that is already very narrow. This is called a thrombotic stroke .
- A clot may break off from another place in the blood vessels of the brain, or from some other part of the body, and travel up to the brain. This is called cerebral embolism, or an embolic stroke .
Ischemic strokes may also be caused by a sticky substance called plaque that can clog arteries.
A hemorrhagic stroke occurs when a blood vessel in part of the brain becomes weak and bursts open. This causes blood to leak into the brain. Some people have defects in the blood vessels of the brain that make this more likely. These defects may include:
-
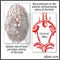
Aneurysm
Aneurysm
An aneurysm is a weak area in the wall of a blood vessel that causes the blood vessel to bulge or balloon out. When an aneurysm occurs in a blood ve...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Arteriovenous malformation
(AVM)
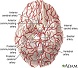
Arteriovenous malformation
A cerebral arteriovenous malformation (AVM) is an abnormal connection between the arteries and veins in the brain that usually forms before birth....
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
Hemorrhagic strokes may also occur when someone is taking blood thinners, such as warfarin (Coumadin). Very high blood pressure may cause blood vessels to burst, leading to hemorrhagic stroke.
An ischemic stroke can develop bleeding and become a hemorrhagic stroke.
High blood pressure is the main risk factor for strokes . Other major risk factors are:
High blood pressure
Blood pressure is a measurement of the force exerted against the walls of your arteries as your heart pumps blood to your body. Hypertension is the ...

Risk factor for strokes
A risk factor is something that increases your chance of getting a disease or health problem. Some risk factors for stroke you cannot change. Some ...
-
Irregular heartbeat, called
atrial fibrillation
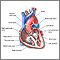
Atrial fibrillation
Atrial fibrillation or flutter is a common type of abnormal heartbeat. The heart rhythm is fast and most often irregular.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Diabetes
Diabetes
Diabetes is a chronic disease in which the body cannot regulate the amount of sugar in the blood.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Family history of stroke
-
High cholesterol
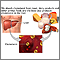
High cholesterol
Cholesterol is a fat (also called a lipid) that your body needs to work properly. Too much bad cholesterol can increase your chance of getting heart...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Increasing age, especially after age 55
- Ethnicity (African Americans are more likely to die of a stroke)
Stroke risk is also higher in:
-
People who have heart disease or
poor blood flow in their legs
caused by narrowed arteries
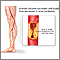
Poor blood flow in their legs
Peripheral artery disease (PAD) is a condition of the blood vessels that supply the legs and feet. It leads to narrowing and hardening of the arteri...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
People who have
unhealthy lifestyle
habits such as smoking, a high-fat diet, and lack of exercise
Unhealthy lifestyle
Good health habits can allow you to avoid illness and improve your quality of life. The following steps will help you feel better and live better. G...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Women who take birth control pills (especially those who smoke and are older than 35)
- Women who are pregnant have an increased risk while pregnant
- Women who take hormone replacement therapy
Symptoms
Symptoms of stroke depend on which part of the brain is damaged. In some cases, a person may not know that a stroke has occurred.
Most of the time, symptoms develop suddenly and without warning. But symptoms may occur on and off for the first day or two. Symptoms are usually most severe when the stroke first happens, but they may slowly get worse.
A headache may occur if the stroke is caused by bleeding in the brain. The headache:
- Starts suddenly and may be severe
- May be worse when you are lying flat
- Wakes you up from sleep
- Gets worse when you change positions or when you bend, strain, or cough
Other symptoms depend on how severe the stroke is, and what part of the brain is affected. Symptoms may include:
- Change in alertness (including sleepiness, unconsciousness, and coma)
- Changes in hearing or taste
- Changes that affect touch and the ability to feel pain, pressure, or different temperatures
- Confusion or loss of memory
- Problems swallowing
- Problems writing or reading
- Dizziness or abnormal feeling of movement (vertigo)
- Eyesight problems, such as decreased vision, double vision, or total loss of vision
- Lack of control over the bladder or bowels
- Loss of balance or coordination, or trouble walking
- Muscle weakness in the face, arm, or leg (usually just on one side)
- Numbness or tingling on one side of the body
- Personality, mood, or emotional changes
- Trouble speaking or understanding others who are speaking
Exams and Tests
The doctor will do a physical exam to:
- Check for problems with vision, movement, feeling, reflexes, understanding, and speaking. Your doctor and nurses will repeat this exam over time to see if your stroke is getting worse or improving.
- Listen to the carotid arteries in the neck with a stethoscope for an abnormal sound, called a bruit, which is caused by abnormal blood flow.
- Check for high blood pressure.
You may have the following tests to help find the type, location, and cause of the stroke and rule out other problems:
-
Angiogram of the head
to look for a blood vessel that is blocked or bleeding
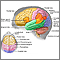
Angiogram of the head
Cerebral angiography is a procedure that uses a special dye (contrast material) and x-rays to see how blood flows through the brain.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Carotid duplex
(ultrasound) to see if the carotid arteries in your neck have narrowed
Carotid duplex
Carotid duplex is an ultrasound test that shows how well blood is flowing through the carotid arteries. The carotid arteries are located in the neck...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Echocardiogram
to see if the stroke could have been caused by a blood clot from the heart
Echocardiogram
An echocardiogram is a test that uses sound waves to create pictures of the heart. The picture and information it produces is more detailed than a s...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Magnetic resonance angiography (
MRA
) or CT angiography to check for abnormal blood vessels in the brain
MRA
Magnetic resonance angiography (MRA) is an MRI exam of the blood vessels. Unlike traditional angiography that involves placing a tube (catheter) int...
Read Article Now Book Mark Article
Other tests include:
- Blood tests
-
Electrocardiogram (
ECG
) and
heart rhythm monitoring
ECG
An electrocardiogram (ECG) is a test that records the electrical activity of the heart.
 ImageRead Article Now Book Mark Article
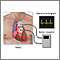
ImageRead Article Now Book Mark ArticleHeart rhythm monitoring
A Holter monitor is a machine that continuously records the heart's rhythms. The monitor is worn for 24 to 48 hours during normal activity.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
Treatment
A stroke is a medical emergency. Quick treatment is needed. Call 9-1-1 or your local emergency number right away or seek urgent medical care at the first signs of a stroke.
People who are having stroke symptoms need to get to a hospital as quickly as possible.
- If the stroke is caused by a blood clot, a clot-busting drug may be given to dissolve the clot.
- To be effective, this treatment must be started within 3 to 4 1/2 hours of when the symptoms first started. The sooner this treatment is started, the better the chance of a good outcome.
Other treatments given in the hospital depend on the cause of the stroke. These may include:
- Blood thinners such as heparin, warfarin (Coumadin), aspirin, or clopidogrel (Plavix)
- Medicine to control risk factors, such as high blood pressure, diabetes, and high cholesterol
- Special procedures or surgery to relieve symptoms or prevent more strokes
- Nutrients and fluids
Physical therapy, occupational therapy, speech therapy, and swallowing therapy will all begin in the hospital. If the person has severe swallowing problems, a feeding tube in the stomach (gastrostomy tube) will likely be needed.
The goal of treatment after a stroke is to help you recover as much function as possible and prevent future strokes.
Recovery from your stroke will begin while you are still in the hospital or at a rehabilitation center. It will continue when you go home from the hospital or center. Be sure to follow up with your health care provider after you go home.
Recovery
A stroke happens when blood flow to any part of the brain stops. Each person has a different recovery time and need for long-term care. Problems wit...
Support Groups
Support and resources are available from the American Stroke Association -- www.strokeassociation.org .
Outlook (Prognosis)
How well a person does after a stroke depends on:
- The type of stroke
- How much brain tissue is damaged
- What body functions have been affected
- How quickly treatment is given
Problems moving, thinking, and talking often improve in the weeks to months after a stroke.
Many people who have had a stroke will keep improving in the months or years after their stroke.
Over half of people who have a stroke are able to function and live at home. Others are not able to care for themselves.
If treatment with clot-busting drugs is successful, the symptoms of a stroke may go away. However, people often do not get to the hospital soon enough to receive these drugs, or they cannot take these drugs because of a health condition.
People who have a stroke from a blood clot (ischemic stroke) have a better chance of surviving than those who have a stroke from bleeding in the brain (hemorrhagic stroke).
The risk for a second stroke is highest during the weeks or months after the first stroke. The risk begins to decrease after this period.
When to Contact a Medical Professional
Stroke is a medical emergency that needs to be treated right away. The acronym F.A.S.T. is an easy way to remember signs of stroke and what to do if you think a stroke has occurred. The most important action to take is to immediately call 911 for emergency assistance.
F.A.S.T. stands for:
- FACE. Ask the person to smile. Check to see if one side of the face droops.
- ARMS. Ask the person to raise both arms. See if one arm drifts downward.
- SPEECH. Ask the person to repeat a simple sentence. Check to see if words are slurred and if the sentence is repeated correctly.
- TIME. If a person shows any of these symptoms, time is essential. It is important to get to the hospital as quickly as possible. Call 911. Act F.A.S.T.
Prevention
Reducing your stroke risk factors lessens your chance of a having stroke.
References
Biller J, Ruland S, Schneck MJ. Ischemic cerebrovascular disease. In Daroff RB, Jankovic J, Mazziotta JC, Pomeroy SL, eds. Bradley's Neurology in Clinical Practice . 7th ed. Philadelphia, PA: Elsevier; 2016:chap 65.
January CT, Wann LS, Alpert JS, et al. 2014 AHA/ACC/HRS Guideline for the management of patients with atrial fibrillation: a report of the American College of Cardiology/American Heart Association Task Force on practice guidelines and the Heart Rhythm Society. Circulation . 2014;130(23):2071-2104. PMID: 24682348 www.ncbi.nlm.nih.gov/pubmed/24682348 .
Jauch EC, Saver JL, Adams Jr HP, et al. Guidelines for the early management of patients with acute ischemic stroke: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke . 2013;44(3):870-947. PMID: 23370205 www.ncbi.nlm.nih.gov/pubmed/23370205 .
Lansberg MG, O'Donnell MJ, Khatri P, et al. Antithrombotic and thrombolytic therapy for ischemic stroke: antithrombotic therapy and prevention of thrombosis, 9th ed: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines. Chest . 2012;141(2 Suppl):e601S-e636S. PMID: 23315273 www.ncbi.nlm.nih.gov/pubmed/22315273 .
Meschia JF, Bushnell C, Boden-Albala B, et al. Guidelines for the primary prevention of stroke: a statement for healthcare professionals from the American Heart Association/American Stroke Association. Stroke . 2014;45(12):3754-3832. PMID: 25355838 www.ncbi.nlm.nih.gov/pubmed/25355838 .
Powers WJ, Derdeyn CP, Biller J, et al. 2015 American Heart Association/American Stroke Association Focused Update of the 2013 Guidelines for the early management of patients with acute ischemic stroke regarding endovascular treatment: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke . 2015;46(10):3020-3035. PMID: 26123479 www.ncbi.nlm.nih.gov/pubmed/26123479 .
-
Hypertension - overview
Animation
-
Stroke
Animation
-
Stroke - secondary to cardiogenic embolism
Animation
-
Stroke
Animation
-
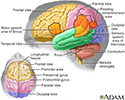
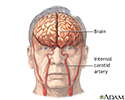
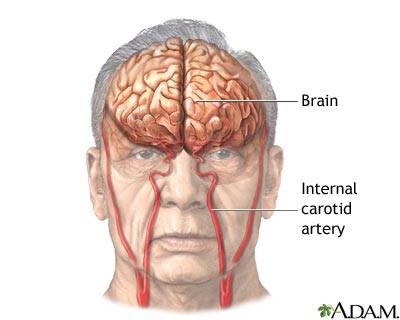
Brain - illustration
The major areas of the brain have one or more specific functions.
Brain
illustration
-
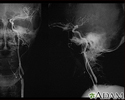
Carotid stenosis, X-ray of the left artery - illustration
A carotid arteriogram is an x-ray study designed to determine if there is narrowing or other abnormality in the carotid artery, a main artery to the brain. This is an angiogram of the left common carotid artery (both front-to-back and side views) showing a severe narrowing (stenosis) of the internal carotid artery just beyond the division of the common carotid artery into the internal and external branches.
Carotid stenosis, X-ray of the left artery
illustration
-
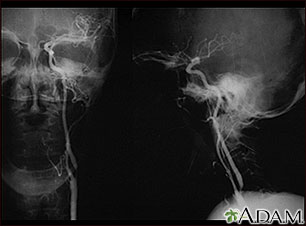
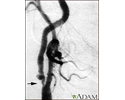
Carotid stenosis, X-ray of the right artery - illustration
This is an angiogram of the right carotid artery showing a severe narrowing (stenosis) of the internal carotid artery just past the carotid fork. There is enlargement of the artery or ulceration in the area after the stenosis in this close-up film. Note the narrowed segment toward the bottom of the picture.
Carotid stenosis, X-ray of the right artery
illustration
-
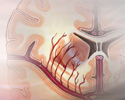
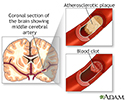
Stroke - illustration
A stroke involves loss of brain functions caused by a loss of blood circulation to areas of the brain. The blockage usually occurs when a clot or piece of atherosclerotic plaque breaks away from another area of the body and lodges within the vasculature of the brain.
Stroke
illustration
-
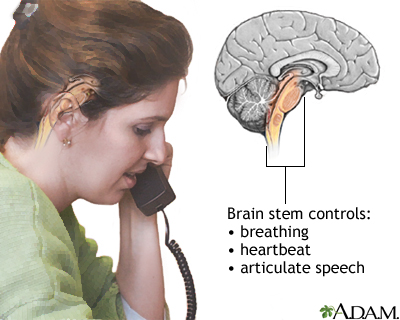
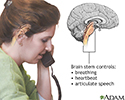
Brainstem function - illustration
A stroke affecting the brain stem is potentially life threatening since this area of the brain controls functions such as breathing and instructing the heart to beat. Brain stem stroke may also cause double vision, nausea and loss of coordination.
Brainstem function
illustration
-
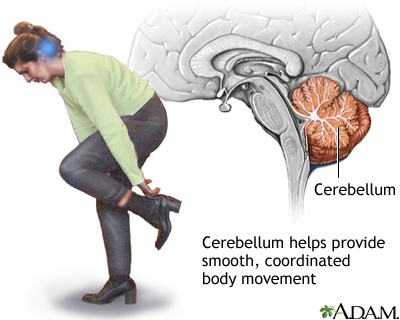
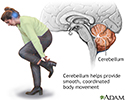
Cerebellum - function - illustration
The cerebellum processes input from other areas of the brain, spinal cord and sensory receptors to provide precise timing for coordinated, smooth movements of the skeletal muscular system. A stroke affecting the cerebellum may cause dizziness, nausea, balance and coordination problems.
Cerebellum - function
illustration
-
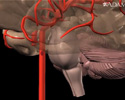
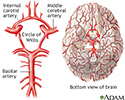
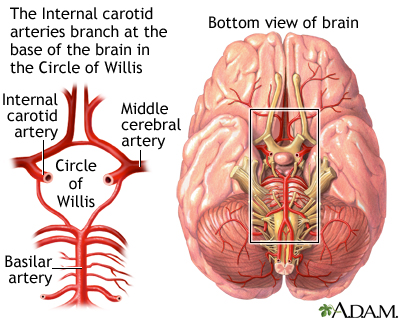
Circle of Willis - illustration
The Circle of Willis is the joining area of several arteries at the bottom (inferior) side of the brain. At the Circle of Willis, the internal carotid arteries branch into smaller arteries that supply oxygenated blood to over 80% of the cerebrum.
Circle of Willis
illustration
-
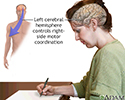
Left cerebral hemisphere - function - illustration
The left cerebral hemisphere controls movement of the right side of the body. Depending on the severity, a stroke affecting the left cerebral hemisphere may result in functional loss or motor skill impairment of the right side of the body, and may also cause loss of speech.
Left cerebral hemisphere - function
illustration
-
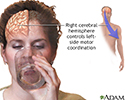
Right cerebral hemisphere - function - illustration
The right cerebral hemisphere controls movement of the left side of the body. Depending on the severity, a stroke affecting the right cerebral hemisphere may result in functional loss or motor skill impairment of the left side of the body. In addition, there may be impairment of the normal attention to the left side of the body and its surroundings.
Right cerebral hemisphere - function
illustration
-
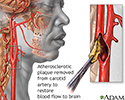
Endarterectomy - illustration
Endarterectomy is a surgical procedure removing plaque material from the lining of an artery.
Endarterectomy
illustration
-
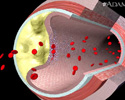
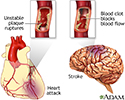
Plaque buildup in arteries - illustration
A heart attack or stroke may occur when an area of plaque (atherosclerosis) ruptures and a clot forms over the location, blocking the flow of blood to the organ's tissues.
Plaque buildup in arteries
illustration
-
Stroke - Series
Presentation
-
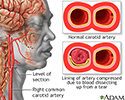
Carotid dissection - illustration
Stroke is defined as a loss of brain function due to blocked blood circulation to the brain. Strokes may be caused by a narrowing, obstruction, or leak in the lining of the carotid. This leaking of blood into the artery wall (dissection) may cause a clot to form, reducing blood flow and raising the risk of a stroke. The leak may arise from an injury to the neck, which means stroke secondary to carotid dissection may occur in young people as well as older people.
Carotid dissection
illustration
-
Hypertension - overview
Animation
-
Stroke
Animation
-
Stroke - secondary to cardiogenic embolism
Animation
-
Stroke
Animation
-
Brain - illustration
The major areas of the brain have one or more specific functions.
Brain
illustration
-
Carotid stenosis, X-ray of the left artery - illustration
A carotid arteriogram is an x-ray study designed to determine if there is narrowing or other abnormality in the carotid artery, a main artery to the brain. This is an angiogram of the left common carotid artery (both front-to-back and side views) showing a severe narrowing (stenosis) of the internal carotid artery just beyond the division of the common carotid artery into the internal and external branches.
Carotid stenosis, X-ray of the left artery
illustration
-
Carotid stenosis, X-ray of the right artery - illustration
This is an angiogram of the right carotid artery showing a severe narrowing (stenosis) of the internal carotid artery just past the carotid fork. There is enlargement of the artery or ulceration in the area after the stenosis in this close-up film. Note the narrowed segment toward the bottom of the picture.
Carotid stenosis, X-ray of the right artery
illustration
-
Stroke - illustration
A stroke involves loss of brain functions caused by a loss of blood circulation to areas of the brain. The blockage usually occurs when a clot or piece of atherosclerotic plaque breaks away from another area of the body and lodges within the vasculature of the brain.
Stroke
illustration
-
Brainstem function - illustration
A stroke affecting the brain stem is potentially life threatening since this area of the brain controls functions such as breathing and instructing the heart to beat. Brain stem stroke may also cause double vision, nausea and loss of coordination.
Brainstem function
illustration
-
Cerebellum - function - illustration
The cerebellum processes input from other areas of the brain, spinal cord and sensory receptors to provide precise timing for coordinated, smooth movements of the skeletal muscular system. A stroke affecting the cerebellum may cause dizziness, nausea, balance and coordination problems.
Cerebellum - function
illustration
-
Circle of Willis - illustration
The Circle of Willis is the joining area of several arteries at the bottom (inferior) side of the brain. At the Circle of Willis, the internal carotid arteries branch into smaller arteries that supply oxygenated blood to over 80% of the cerebrum.
Circle of Willis
illustration
-
Left cerebral hemisphere - function - illustration
The left cerebral hemisphere controls movement of the right side of the body. Depending on the severity, a stroke affecting the left cerebral hemisphere may result in functional loss or motor skill impairment of the right side of the body, and may also cause loss of speech.
Left cerebral hemisphere - function
illustration
-
Right cerebral hemisphere - function - illustration
The right cerebral hemisphere controls movement of the left side of the body. Depending on the severity, a stroke affecting the right cerebral hemisphere may result in functional loss or motor skill impairment of the left side of the body. In addition, there may be impairment of the normal attention to the left side of the body and its surroundings.
Right cerebral hemisphere - function
illustration
-
Endarterectomy - illustration
Endarterectomy is a surgical procedure removing plaque material from the lining of an artery.
Endarterectomy
illustration
-
Plaque buildup in arteries - illustration
A heart attack or stroke may occur when an area of plaque (atherosclerosis) ruptures and a clot forms over the location, blocking the flow of blood to the organ's tissues.
Plaque buildup in arteries
illustration
-
Stroke - Series
Presentation
-
Carotid dissection - illustration
Stroke is defined as a loss of brain function due to blocked blood circulation to the brain. Strokes may be caused by a narrowing, obstruction, or leak in the lining of the carotid. This leaking of blood into the artery wall (dissection) may cause a clot to form, reducing blood flow and raising the risk of a stroke. The leak may arise from an injury to the neck, which means stroke secondary to carotid dissection may occur in young people as well as older people.
Carotid dissection
illustration
Review Date: 7/7/2015
Reviewed By: Daniel Kantor, MD, Kantor Neurology, Coconut Creek, FL and Immediate Past President of the Florida Society of Neurology (FSN), Gainesville, FL. Review provided by VeriMed Healthcare Network. Internal review and update on 07/24/2016 by David Zieve, MD, MHA, Isla Ogilvie, PhD, and the A.D.A.M. Editorial team.