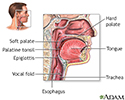
Stuffy or runny nose - adult
Nose - congested; Congested nose; Runny nose; Postnasal drip; Rhinorrhea: nasal congestion
A stuffy or congested nose occurs when the tissues lining it become swollen. The swelling is due to inflamed blood vessels.
The problem may also include nasal discharge or "runny nose." If excess mucus runs down the back of your throat (postnasal drip), it may cause a cough or sore throat.
Causes
A stuffy or runny nose may be caused by:
-
Common cold
Common cold
The common cold most often causes a runny nose, nasal congestion, and sneezing. You may also have a sore throat, cough, headache, or other symptoms....
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Flu
Flu
The flu is an infection of the nose, throat, and lungs. It spreads easily. This article discusses influenza types A and B. Another type of the flu ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Sinus infection
Sinus infection
Sinusitis is present when the tissue lining the sinuses become swollen or inflamed. It occurs as the result of an infection from a virus, bacteria, ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
The congestion typically goes away by itself within a week.
Congestion also can be caused by:
-
Hay fever
or other allergies
Hay fever
Allergic rhinitis is a diagnosis associated with a group of symptoms affecting the nose. These symptoms occur when you breathe in something you are ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Use of some nasal sprays or drops bought without a prescription for more than 3 days (may make nasal stuffiness worse)
-
Nasal polyps
, sac-like growths of inflamed tissue lining the nose or sinuses
Nasal polyps
Nasal polyps are soft, sac-like growths on the lining of the nose or sinuses.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Pregnancy
-
Vasomotor rhinitis
Vasomotor rhinitis
Rhinitis is a condition that includes a runny nose, sneezing, and nasal stuffiness. When hay fever or allergies are not causing these symptoms, the ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
Home Care
Finding ways to keep mucus thin will help it drain from your nose and sinuses and relieve your symptoms. Drinking plenty of clear fluids is one way to do this. You can also:
- Apply a warm, moist washcloth to your face several times a day.
- Inhale steam 2 to 4 times a day. One way to do this is to sit in the bathroom with the shower running. Do not inhale hot steam.
- Use a vaporizer or humidifier.
A nasal wash can help remove mucus from your nose.
- You can buy a saline spray at a drugstore or make one at home. To make one, use 1 cup (240 milliliters) of warm water, 1/2 teaspoon (3 grams) of salt, and a pinch of baking soda.
- Use gentle saline nasal sprays 3 to 4 times per day.
Congestion is often worse when lying down. Keep upright, or at least keep the head elevated.
Some stores sell adhesive strips that can be placed on the nose. These help widen the nostrils, making breathing easier.
Medicines you can buy at the store without a prescription can help your symptoms.
- Decongestants are drugs that shrink and dry up your nasal passages. They may help dry up a runny or stuffy nose.
-
Antihistamines
are drugs that treat allergy symptoms. Some antihistamines make you drowsy so use with care.
Antihistamines
Antihistamines are drugs that treat allergy symptoms. When taken by mouth, they come as pills, chewable tablets, capsules, and liquids.
Read Article Now Book Mark Article - Nasal sprays can relieve stuffiness. Don't use over-the-counter nasal sprays more often than 3 days on and 3 days off, unless told to by your health care provider.
Many cough, allergy, and cold medicines you buy have more than one medicine inside. Read the labels carefully to make sure you don't take too much of any 1 medicine. Ask your provider which cold medicines are safe for you
If you have allergies:
- Your provider may also prescribe nasal sprays that treat allergy symptoms.
-
Learn how to avoid triggers that make
allergies worse
.
Allergies worse
Hay fever - self-care; Seasonal rhinitis - self-care; Allergies - allergic rhinitis - self-care
Read Article Now Book Mark Article
When to Contact a Medical Professional
Call your provider for any of the following:
- A stuffy nose with swelling of the forehead, eyes, side of the nose, or cheek, or that occurs with blurred vision
- More throat pain, or white or yellow spots on the tonsils or other parts of the throat
- Discharge from the nose that has a bad smell, comes from only one side, or is a color other than white or yellow
- Cough that lasts longer than 10 days, or produces yellow-green or gray mucus
- Nasal discharge following a head injury
- Symptoms that last more than 3 weeks
- Nasal discharge with fever
What to Expect at Your Office Visit
Your provider may perform a physical exam that focuses on the ears, nose, throat, and airways.
Tests that may be done include:
-
Allergy
skin and blood tests
Allergy
An allergy is an immune response or reaction to substances that are usually not harmful.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Blood tests
-
Sputum culture
and
throat culture
Sputum culture
Routine sputum culture is a laboratory test that looks for germs that cause infection. Sputum is the material that comes up from air passages when y...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark ArticleThroat culture
A throat swab culture is a laboratory test that is done to identify germs that may cause infection in the throat. It is most often used to diagnose ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
X-rays of the sinuses
and
chest x-ray
X-rays of the sinuses
A skull x-ray is a picture of the bones surrounding the brain, including the facial bones, the nose, and the sinuses.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark ArticleChest x-ray
A chest x-ray is an x-ray of the chest, lungs, heart, large arteries, ribs, and diaphragm.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
References
Bachert C, Calus L, Gevaert P. Rhinosinusitis and nasal polyps. In: Adkinson NF, Bochner BS, Burks AW, et al, eds. Middleton's Allergy: Principles and Practice . 8th ed. Philadelphia, PA: Elsevier Saunders; 2014:chap 43.
Corren J, Baroody FM, Pawankar R. Allergic and nonallergic rhinitis. In: Adkinson NF, Bochner BS, Burks AW, et al, eds. Middleton's Allergy: Principles and Practice . 8th ed. Philadelphia, PA: Elsevier Saunders; 2014:chap 42.
Review Date: 8/14/2015
Reviewed By: Linda J. Vorvick, MD, Medical Director and Director of Didactic Curriculum, MEDEX Northwest Division of Physician Assistant Studies, Department of Family Medicine, UW Medicine, School of Medicine, University of Washington, Seattle, WA. Also reviewed by David Zieve, MD, MHA, Isla Ogilvie, PhD, and the A.D.A.M. Editorial team.