Heartburn
Pyrosis; Non-cardiac chest pain
Heartburn is a painful burning feeling just below or behind the breastbone. Most of the time it comes from the esophagus. The pain often rises in your chest from your stomach. It may also spread to your neck or throat.
Causes
Almost everyone has heartburn sometimes. If you have heartburn very often, you may have gastroesophageal reflux disease (GERD).
Gastroesophageal reflux disease
Gastroesophageal reflux disease (GERD) is a condition in which the stomach contents leak backwards from the stomach into the esophagus (the tube from...
Normally when food or liquid enters your stomach, a band of muscle at the end of your esophagus closes off the esophagus. This band is called the lower esophageal sphincter (LES). If this band does not close tightly enough, food or stomach acid can back up (reflux) into the esophagus. The stomach contents can irritate the esophagus and cause heartburn and other symptoms.
Heartburn is more likely if you have a hiatal hernia . A hiatal hernia is a conditions which occurs when the top part of the stomach pokes into the chest cavity. This weakens the LES so that it is easier for acid to back up from the stomach into the esophagus.
Hiatal hernia
Hiatal hernia is a condition in which part of the stomach extends through an opening of the diaphragm into the chest. The diaphragm is the sheet of ...
Pregnancy and many medicines can bring on heartburn or make it worse.
Medicines that can cause heartburn include:
- Anticholinergics (used for sea sickness)
- Beta-blockers for high blood pressure or heart disease
- Calcium channel blockers for high blood pressure
- Dopamine-like drugs for Parkinson disease
- Progestin for abnormal menstrual bleeding or birth control
- Sedatives for anxiety or sleep problems (insomnia)
- Theophylline (for asthma or other lung diseases)
- Tricyclic antidepressants
Talk to your health care provider if you think one of your medicines may be causing heartburn. Never change or stop taking medicine without talking to your provider first.
Home Care
You should treat heartburn because reflux can damage the lining of your esophagus. This can cause serious problems over time. Changing your habits can be helpful in preventing heartburn and other symptoms of GERD.
The following tips will help you avoid heartburn and other GERD symptoms. Talk to your provider if you are still bothered by heartburn after trying these steps.
First, avoid foods and drinks that can trigger reflux, such as:
- Alcohol
- Caffeine
- Carbonated drinks
- Chocolate
- Citrus fruits and juices
- Peppermint and spearmint
- Spicy or fatty foods, full-fat dairy products
- Tomatoes and tomato sauces
Next, try changing your eating habits:
- Avoid bending over or exercising just after eating.
- Avoid eating within 3 to 4 hours of bedtime. Lying down with a full stomach causes the stomach contents to press harder against the lower esophageal sphincter (LES).
- Eat smaller meals.
Make other lifestyle changes as needed:
- Avoid tight-fitting belts or clothes that are snug around the waist. These items can squeeze the stomach, and may force food to reflux.
- Lose weight if you are overweight. Obesity increases pressure in the stomach. This pressure can push the stomach contents into the esophagus. In some cases, GERD symptoms go away after an overweight person loses 10 to 15 pounds (4.5 to 6.75 kilograms).
- Sleep with your head raised about 6 inches (15 centimeters). Sleeping with the head higher than the stomach helps prevent digested food from backing up into the esophagus. Place books, bricks, or blocks under the legs at the head of your bed. You can also use a wedge-shaped pillow under your mattress. Sleeping on extra pillows does NOT work well for relieving heartburn because you can slip off the pillows during the night.
- Stop smoking. Chemicals in cigarette smoke weaken the LES.
- Reduce stress. Try yoga, tai chi, or meditation to help relax.
If you still do not have full relief, try over-the-counter medicines:
- Antacids, like Maalox, Mylanta, or Tums help neutralize stomach acid.
- H2 blockers, like Pepcid AC, Tagamet, and Zantac, reduce stomach acid production.
- Proton pump inhibitors, like Prilosec OTC, stop nearly all stomach acid production.
When to Contact a Medical Professional
Get urgent medical care if:
- You vomit material that is bloody or looks like coffee grounds.
-
Your
stools are black
(like tar) or maroon.
Stools are black
Bloody stools often are a sign of a problem in the digestive tract. Blood in the stool may come from anywhere along your digestive tract from your m...
Read Article Now Book Mark Article - You have a burning feeling and a squeezing, crushing, or pressure in your chest. Sometimes people who think they have heartburn are having a heart attack.
Call your health care provider if:
- You have heartburn often or it does not go away after a few weeks of self-care.
- You lose weight that you did not want to lose.
- You have trouble swallowing (food feels stuck as it goes down).
- You have a cough or wheezing that does not go away.
- Your symptoms get worse with antacids, H2 blockers, or other treatments.
You think one of your medicines may be causing heartburn. DO NOT change or stop taking your medicine on your own.
What to Expect at Your Office Visit
Heartburn is easy to diagnose from your symptoms in most cases. Sometimes, heartburn can be confused with another stomach problem called dyspepsia. If the diagnosis is unclear, you may be sent to a doctor called a gastroenterologist for more testing.
First, your provider will do a physical exam and ask questions about your heartburn, such as:
- When did it begin?
- How long does each episode last?
- Is this the first time you have had heartburn?
- What do you usually eat at each meal? Before you feel heartburn, have you eaten a spicy or fatty meal?
- Do you drink a lot of coffee, other drinks with caffeine, or alcohol? Do you smoke?
- Do you wear clothing that is tight in the chest or belly?
- Do you also have pain in the chest, jaw, arm, or somewhere else?
- What medicines are you taking?
- Have you vomited blood or black material?
-
Do you have
blood in your stools
?
Blood in your stools
Bloody stools often are a sign of a problem in the digestive tract. Blood in the stool may come from anywhere along your digestive tract from your m...
Read Article Now Book Mark Article -
Do you have
black, tarry stools
?
Black, tarry stools
Bloody stools often are a sign of a problem in the digestive tract. Blood in the stool may come from anywhere along your digestive tract from your m...
Read Article Now Book Mark Article - Are there other symptoms with your heartburn?
You may need the following tests:
-
Esophageal motility
to measure the pressure of your LES
Esophageal motility
Esophageal manometry is a test to measure how well the esophagus is working.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Esophagogastroduodenoscopy
(upper endoscopy) to look at the inside lining of your esophagus and stomach
Esophagogastroduodenoscopy
Esophagogastroduodenoscopy (EGD) is a test to examine the lining of the esophagus, stomach, and first part of the small intestine.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Upper GI series
Upper GI series
An upper GI and small bowel series is a set of x-rays taken to examine the esophagus, stomach, and small intestine. Barium enema is a related test....
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
If your symptoms do not get better with home care, you may need to take medicine to reduce acid that is stronger than over-the-counter medicines. Any sign of bleeding will need more testing and treatment.
References
Falk GW, Katzka DA. Diseases of the esophagus. In: Goldman L, Schafer AI, eds. Goldman's Cecil Medicine . 24th ed. Philadelphia, PA: Elsevier Saunders; 2011:chap 140.
Katz PO, Gerson LB, Vela MF. Diagnosis and Management of Gastroesophageal Reflux Disease. Am J Gastroenterol . 2013;108:308-28. PMID: 23419381 www.ncbi.nlm.nih.gov/pubmed/23419381 .
-
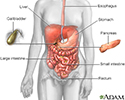
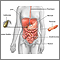
Digestive system - illustration
The esophagus, stomach, large and small intestine, aided by the liver, gallbladder and pancreas convert the nutritive components of food into energy and break down the non-nutritive components into waste to be excreted.
Digestive system
illustration
-
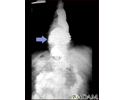
Hiatal hernia - X-ray - illustration
This x-ray shows the upper portion of the stomach protruding through the diaphragm (hiatal hernia).
Hiatal hernia - X-ray
illustration
-
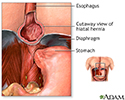
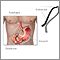
Hiatal hernia - illustration
A hiatal hernia occurs when part of the stomach protrudes up into the chest through the sheet of muscle called the diaphragm. This may result from a weakening of the surrounding tissues and may be aggravated by obesity and/or smoking.
Hiatal hernia
illustration
-
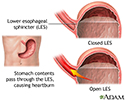
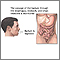
Gastroesophageal reflux disease - illustration
A band of muscle fibers, the lower esophageal sphincter, closes off the esophagus from the stomach. If the sphincter does not close properly, food and liquid can move backward into the esophagus and cause heartburn and other symptoms known as gastroesophageal disease (GERD). To alleviate symptoms dietary changes and medications are prescribed. For a patient who has persistent symptoms despite medical treatment, an anti-reflux operation may be an option.
Gastroesophageal reflux disease
illustration
-
Digestive system - illustration
The esophagus, stomach, large and small intestine, aided by the liver, gallbladder and pancreas convert the nutritive components of food into energy and break down the non-nutritive components into waste to be excreted.
Digestive system
illustration
-
Hiatal hernia - X-ray - illustration
This x-ray shows the upper portion of the stomach protruding through the diaphragm (hiatal hernia).
Hiatal hernia - X-ray
illustration
-
Hiatal hernia - illustration
A hiatal hernia occurs when part of the stomach protrudes up into the chest through the sheet of muscle called the diaphragm. This may result from a weakening of the surrounding tissues and may be aggravated by obesity and/or smoking.
Hiatal hernia
illustration
-
Gastroesophageal reflux disease - illustration
A band of muscle fibers, the lower esophageal sphincter, closes off the esophagus from the stomach. If the sphincter does not close properly, food and liquid can move backward into the esophagus and cause heartburn and other symptoms known as gastroesophageal disease (GERD). To alleviate symptoms dietary changes and medications are prescribed. For a patient who has persistent symptoms despite medical treatment, an anti-reflux operation may be an option.
Gastroesophageal reflux disease
illustration
-
Gastroesophageal reflux disease and heartburn
(In-Depth)
-
Gastroesophageal reflux disease
(Alt. Medicine)
Review Date: 1/11/2015
Reviewed By: Todd Eisner, MD, Private practice specializing in Gastroenterology, and Affiliate Assistant Professor, Florida Atlantic University School of Medicine, Boca Raton, FL. Review provided by VeriMed Healthcare Network. Also reviewed by David Zieve, MD, MHA, Isla Ogilvie, PhD, and the A.D.A.M. Editorial team.