Movement - uncoordinated
Lack of coordination; Loss of coordination; Coordination impairment; Ataxia; Clumsiness; Uncoordinated movement
Uncoordinated movement is due to a muscle control problem that causes an inability to coordinate movements. It leads to a jerky, unsteady, to-and-fro motion of the middle of the body (trunk) and an unsteady gait (walking style). It can also affect the limbs.
Unsteady gait
Walking abnormalities are unusual and uncontrollable walking patterns. They are usually due to diseases or injuries to the legs, feet, brain, spinal...
The medical name of this condition is ataxia.
Considerations
Smooth graceful movement requires a balance between different muscle groups. A part of the brain called the cerebellum manages this balance.
Causes
Diseases that damage the cerebellum, spinal cord, or peripheral nerves can interfere with normal muscle movement. The result is large, jerky, uncoordinated movements.
Peripheral
Peripheral means "away from the center. " It refers to areas away from the center of the body or a body part. For example, the hands are peripheral ...

Brain injuries or diseases that can cause uncoordinated movements include:
- Brain injury or head trauma
-
Chickenpox
or certain other brain infections (
encephalitis
)
Chickenpox
Chickenpox is a viral infection in which a person develops very itchy blisters all over the body. It was more common in the past. The illness is ra...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark ArticleEncephalitis
Encephalitis is irritation and swelling (inflammation) of the brain, most often due to infections.
Read Article Now Book Mark Article -
Conditions that are passed through families (such as congenital cerebellar ataxia,
Friedreich ataxia
,
ataxia - telangiectasia
, or
Wilson disease
)
Friedreich ataxia
Friedreich ataxia is a rare disease passed down through families (inherited). It affects the muscles and heart.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark ArticleAtaxia - telangiectasia
Ataxia-telangiectasia is a rare childhood disease. It affects the brain and other parts of the body. Ataxia refers to uncoordinated movements, such ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark ArticleWilson disease
Wilson disease is an inherited disorder in which there is too much copper in the body's tissues. The excess copper damages the liver and nervous sys...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Multiple sclerosis
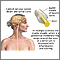
Multiple sclerosis
Multiple sclerosis is an autoimmune disease that affects the brain and spinal cord (central nervous system).
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
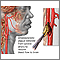
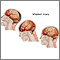
Stroke
or
transient ischemic attack
(TIA)
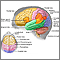
Stroke
A stroke occurs when blood flow to a part of the brain stops. A stroke is sometimes called a "brain attack. " If blood flow is cut off for longer th...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark ArticleTransient ischemic attack
A transient ischemic attack occurs when blood flow to a part of the brain stops for a brief time. A person will have stroke-like symptoms for up to ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
Poisoning or toxic effects caused by:
- Alcohol
- Certain medicines
- Heavy metals such as mercury, thallium, and lead
- Solvents such as toluene or carbon tetrachloride
Other causes include:
- Certain cancers, in which uncoordinated movement symptoms may appear months or years before the cancer is diagnosed (called paraneoplastic syndrome)
- Problems with the nerves in the legs (neuropathy)
- Spine injury or disease causing damage to the spinal cord (such as compression fractures of the spine)
Home Care
A home safety evaluation by a physical therapist may be helpful.
Take steps to make it easier and safer to move around at home. For example, get rid of clutter, leave wide walkways, and remove throw rugs or other objects that might cause slipping or falling.
People with this condition should be encouraged to take part in normal activities. Family members need to be patient with a person who has poor coordination. Take time to show the person ways to do tasks more easily. Take advantage of the person's strengths while avoiding his or her weaknesses.
Ask the health care provider whether walking aids, such as a cane or walker, would be helpful.
When to Contact a Medical Professional
Call your health care provider if:
- A person has unexplained problems with coordination
- Lack of coordination lasts longer than a few minutes
What to Expect at Your Office Visit
In an emergency, the patient will first be stabilized so that symptoms do not get worse.
The health care provider will perform a physical exam, which may include:
- A detailed examination of the nervous system and muscles, paying careful attention to walking, balance, and coordination of pointing with fingers and toes.
- The patient will be asked to stand up with the feet together and the eyes closed. This is called the Romberg test. If the patient loses balance, this is a sign that the sense of position has been lost. In this case, the test is considered positive.
Medical history questions may include:
- When did the symptoms begin?
- Does the uncoordinated movement happen all the time or does it come and go?
- Is it getting worse?
- What medicines do you take?
- Do you drink alcohol?
- Do you use recreational drugs?
- Have you been exposed to something that may have caused poisoning?
-
What other symptoms do you have? For example:
weakness
or
paralysis
,
numbness
, tingling, or loss of sensation,
confusion
or disorientation,
seizures
.
Paralysis
Muscle function loss is when a muscle does not work or move normally. The medical term for complete loss of muscle function is paralysis.
Read Article Now Book Mark ArticleNumbness
Numbness and tingling are abnormal sensations that can occur anywhere in your body, but they are often felt in your fingers, hands, feet, arms, or le...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark ArticleConfusion
Confusion is the inability to think as clearly or quickly as you normally do. You may feel disoriented and have difficulty paying attention, remembe...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark ArticleSeizures
A seizure is the physical findings or changes in behavior that occur after an episode of abnormal electrical activity in the brain. The term "seizure...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
Tests that may be ordered include:
- Antibody testing to check for paraneoplastic syndromes
-
Blood tests (such as a
CBC
or
blood differential
)
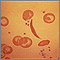
CBC
A complete blood count (CBC) test measures the following:The number of red blood cells (RBC count)The number of white blood cells (WBC count)The tota...
 ImageRead Article Now Book Mark Article
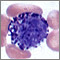
ImageRead Article Now Book Mark ArticleBlood differential
The blood differential test measures the percentage of each type of white blood cell (WBC) that you have in your blood. It also reveals if there are...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
CT scan of the head
CT scan of the head
A head computed tomography (CT) scan uses many x-rays to create pictures of the head, including the skull, brain, eye sockets, and sinuses.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Genetic testing
-
MRI of the head
MRI of the head
A head MRI (magnetic resonance imaging) is an imaging test that uses powerful magnets and radio waves to create pictures of the brain and surrounding...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
You may need to be referred to a specialist for diagnosis and treatment. If a specific problem is causing the ataxia, the problem will be treated. For example, if a medicine is causing coordination problems, the medicine may be changed or stopped. Other causes may not be treatable. The health care provider can tell you more.
References
Lang AE. Other movement disorders. In: Goldman L, Schafer AI, eds. Goldman's Cecil Medicine . 25th ed. Philadelphia, PA: Elsevier Saunders; 2016:chap 410.
Subramony SH. Ataxic disorders and cerebellar disorders. In: Daroff RB, Fenichel GM, Jankovic J, Mazziotta JC, eds. Bradley's Neurology in Clinical Practice. 6th ed. Philadelphia, PA: Elsevier Saunders; 2012:chap 22.
-
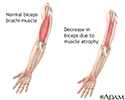
Muscular atrophy - illustration
Muscular atrophy is the decrease in size and wasting of muscle tissue. Muscles that lose their nerve supply can atrophy and simply waste away.
Muscular atrophy
illustration
Review Date: 2/3/2015
Reviewed By: Amit M. Shelat, DO, FACP, Attending Neurologist and Assistant Professor of Clinical Neurology, SUNY Stony Brook, School of Medicine, Stony Brook, NY. Review provided by VeriMed Healthcare Network. Also reviewed by David Zieve, MD, MHA, Isla Ogilvie, PhD, and the A.D.A.M. Editorial team.