West Nile virus
West Nile virus is a disease spread by mosquitoes. The condition ranges from mild to severe.
Causes
West Nile virus was first identified in 1937 in Uganda in eastern Africa. It was first discovered in the U.S. in the summer of 1999 in New York. Since then, the virus has spread throughout the U.S.
Researchers believe West Nile virus is spread when a mosquito bites an infected bird and then bites a person.
Mosquitoes carry the highest amounts of virus in the early fall, which is why more people get the disease in late August to early September. As the weather becomes colder and mosquitoes die off, there are fewer cases of the disease.
Although many people are bitten by mosquitoes that carry West Nile virus, most do not know they have been infected.
Risk factors for developing a more severe form of West Nile virus include:
-
Conditions that weaken the immune system, such as HIV/AIDS, organ transplants, and recent
chemotherapy
Chemotherapy
The term chemotherapy is used to describe cancer-killing drugs. Chemotherapy may be used to:Cure the cancerShrink the cancerPrevent the cancer from ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Older or very young age
- Pregnancy
West Nile virus may also be spread through blood transfusions and organ transplants. It is possible for an infected mother to spread the virus to her child through breast milk.
Symptoms
Symptoms may occur 1 to 14 days after becoming infected. Mild disease, generally called West Nile fever, may cause some or all of the following symptoms:
- Abdominal pain
- Fever, headache, and sore throat
- Lack of appetite
-
Muscle aches
Muscle aches
Muscle aches and pains are common and can involve more than 1 muscle. Muscle pain also can involve ligaments, tendons, and fascia. Fascia are the s...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Nausea, vomiting, and diarrhea
- Rash
- Swollen lymph nodes
These symptoms usually last for 3 to 6 days, but may last a month.
More severe forms of disease are called West Nile encephalitis or West Nile meningitis, depending on what part of the body is affected. The following symptoms can occur, and need prompt attention:
-
Confusion
or change in ability to think clearly
Confusion
Confusion is the inability to think as clearly or quickly as you normally do. You may feel disoriented and have difficulty paying attention, remembe...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Loss of consciousness
or coma
Loss of consciousness
Decreased alertness is a state of reduced awareness. A coma is a state of decreased alertness from which a person cannot be awakened. A long-term co...
Read Article Now Book Mark Article -
Muscle weakness
Muscle weakness
Weakness is reduced strength in one or more muscles.
Read Article Now Book Mark Article - Stiff neck
- Weakness of one arm or leg
Exams and Tests
Signs of West Nile virus infection are similar to those of other viral infections. There may be no specific findings on a physical examination. About half of people with West Nile virus infection may have a rash.
Tests to diagnose West Nile virus include:
-
Blood test or a
spinal tap
to check for
antibodies
against the virus
Spinal tap
Cerebrospinal fluid (CSF) collection is a test to look at the fluid that surrounds the brain and spinal cord. CSF acts as a cushion, protecting the b...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark ArticleAntibodies
An antibody is a protein produced by the body's immune system when it detects harmful substances, called antigens. Examples of antigens include micr...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Head CT scan
Head CT scan
A head computed tomography (CT) scan uses many x-rays to create pictures of the head, including the skull, brain, eye sockets, and sinuses.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Head MRI scan
Head MRI scan
A head MRI (magnetic resonance imaging) is an imaging test that uses powerful magnets and radio waves to create pictures of the brain and surrounding...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
Treatment
Because this illness is not caused by bacteria, antibiotics do not treat West Nile virus infection. Supportive care may help decrease the risk of complications in severe illness.
Outlook (Prognosis)
People with mild West Nile virus infection do well after treatment.
For those with severe infection, the outlook is more uncertain. West Nile encephalitis or meningitis may lead to brain damage and death. 1 in 10 people with brain inflammation do not survive.
Possible Complications
Complications from mild West Nile virus infection are very rare.
Complications from severe West Nile virus infection include:
- Brain damage
-
Permanent muscle weakness (sometimes similar to
polio
)
Polio
Polio is a viral disease that can affect nerves and can lead to partial or full paralysis. The medical name for polio is poliomyelitis.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Death
When to Contact a Medical Professional
Call your health care provider if you have symptoms of West Nile virus infection, especially if you may have had contact with mosquitoes. If you are very sick, go to an emergency room.
There is no treatment to avoid getting West Nile virus infection after a mosquito bite. People in good health generally do not develop a serious West Nile infection.
Prevention
The best way to prevent West Nile virus infection is to avoid mosquito bites:
- Use mosquito-repellant products containing DEET
- Wear long sleeves and pants
- Drain pools of standing water, such as trash bins and plant saucers (mosquitos breed in stagnant water)
Community spraying for mosquitoes may also reduce mosquito breeding.
References
Fischer M, Staples JE, Campbell GL. West Nile virus. In: Magill AJ, Hill DR, Solomon T, Ryan ET, eds. Hunter's Tropical Medicine and Emerging Infectious Diseases . 9th ed. Philadelphia, PA: Elsevier; 2013:chap 34.5.
-
Mosquito, adult feeding on the skin - illustration
There are many different species of mosquito, which can carry some of the world's most common and significant infectious diseases, including West Nile, Malaria, yellow fever, viral encephalitis, and dengue fever. (Image courtesy of the Centers for Disease Control and Prevention.)
Mosquito, adult feeding on the skin
illustration
-
Mosquito, adult - illustration
This illustration shows an adult southern house mosquito. This mosquito feeds on blood and is the carrier of many diseases, such as encephalitis, West Nile, dengue fever, yellow fever, and others. (Image courtesy of the Centers for Disease Control and Prevention.)
Mosquito, adult
illustration
-
Mosquito, egg raft - illustration
Mosquitoes of the Culex species lay their eggs in the form of egg rafts that float in still or stagnant water. The mosquito lays the eggs one at a time sticking them together in the shape of a raft. An egg raft can contain from 100 - 400 eggs. The eggs go through larval and pupal stages and feed on micro-organisms before developing into flying mosquitoes. (Image courtesy of the Centers for Disease Control and Prevention.)
Mosquito, egg raft
illustration
-
Mosquito, pupa - illustration
These are mosquito pupa. This is another stage in the development of the mosquito. (Image courtesy of the Centers for Disease Control and Prevention.)
Mosquito, pupa
illustration
-
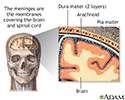
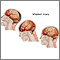
Meninges of the brain - illustration
The organs of the central nervous system (brain and spinal cord) are covered by connective tissue layers collectively called the meninges. Consisting of the pia mater (closest to the CNS structures), the arachnoid and the dura mater (farthest from the CNS), the meninges also support blood vessels and contain cerebrospinal fluid. These are the structures involved in meningitis, an inflammation of the meninges, which, if severe, may become encephalitis, an inflammation of the brain.
Meninges of the brain
illustration
-
Mosquito, adult feeding on the skin - illustration
There are many different species of mosquito, which can carry some of the world's most common and significant infectious diseases, including West Nile, Malaria, yellow fever, viral encephalitis, and dengue fever. (Image courtesy of the Centers for Disease Control and Prevention.)
Mosquito, adult feeding on the skin
illustration
-
Mosquito, adult - illustration
This illustration shows an adult southern house mosquito. This mosquito feeds on blood and is the carrier of many diseases, such as encephalitis, West Nile, dengue fever, yellow fever, and others. (Image courtesy of the Centers for Disease Control and Prevention.)
Mosquito, adult
illustration
-
Mosquito, egg raft - illustration
Mosquitoes of the Culex species lay their eggs in the form of egg rafts that float in still or stagnant water. The mosquito lays the eggs one at a time sticking them together in the shape of a raft. An egg raft can contain from 100 - 400 eggs. The eggs go through larval and pupal stages and feed on micro-organisms before developing into flying mosquitoes. (Image courtesy of the Centers for Disease Control and Prevention.)
Mosquito, egg raft
illustration
-
Mosquito, pupa - illustration
These are mosquito pupa. This is another stage in the development of the mosquito. (Image courtesy of the Centers for Disease Control and Prevention.)
Mosquito, pupa
illustration
-
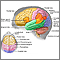
Meninges of the brain - illustration
The organs of the central nervous system (brain and spinal cord) are covered by connective tissue layers collectively called the meninges. Consisting of the pia mater (closest to the CNS structures), the arachnoid and the dura mater (farthest from the CNS), the meninges also support blood vessels and contain cerebrospinal fluid. These are the structures involved in meningitis, an inflammation of the meninges, which, if severe, may become encephalitis, an inflammation of the brain.
Meninges of the brain
illustration
-
Viral encephalitis
(In-Depth)
Review Date: 12/7/2014
Reviewed By: Jatin M. Vyas, MD, PhD, Assistant Professor in Medicine, Harvard Medical School; Assistant in Medicine, Division of Infectious Disease, Department of Medicine, Massachusetts General Hospital, Boston, MA. Also reviewed by David Zieve, MD, MHA, Isla Ogilvie, PhD, and the A.D.A.M. Editorial team.