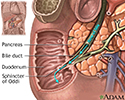
Pancreatic cancer
Pancreatic cancer; Cancer - pancreas
Pancreatic cancer is cancer that starts in the pancreas.
Causes
The pancreas is a large organ behind the stomach. It makes and releases enzymes into the intestines that help the body digest and absorb food, especially fats. The pancreas also makes and releases insulin and glucagon. These are hormones that help the body control blood sugar levels.
There are different types of pancreatic cancers. The type depends on the cell the cancer develops in. Examples include:
- Adenocarcinoma, the most common type of pancreatic cancer
-
Other more rare types include
glucagonoma
,
insulinoma
,
islet cell tumor
,
VIPoma
Glucagonoma
Glucagonoma is a very rare tumor of the islet cells of the pancreas, which leads to an excess of the hormone glucagon in the blood.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark ArticleInsulinoma
An insulinoma is a tumor in the pancreas that produces too much insulin.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark ArticleIslet cell tumor
A pancreatic islet cell tumor is a rare tumor of the pancreas that starts from a type of cell called the islet cell.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark ArticleVIPoma
VIPoma is a very rare cancer that usually grows from cells in the pancreas called islet cells.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
The exact cause of pancreatic cancer is unknown. It is more common in persons who:
- Are obese
- Have a diet high in fat and low in fruits and vegetables
- Have diabetes
- Have long-term exposure to certain chemicals
-
Have long-term inflammation of the pancreas (
chronic pancreatitis
)
Chronic pancreatitis
Pancreatitis is swelling of the pancreas. Chronic pancreatitis is present when this problem does not heal or improve, gets worse over time, and lead...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Smoke
Pancreatic cancer is slightly more common in women than in men. The risk increases with age. Family history of the disease also slightly increases the chance of developing this cancer.
Symptoms
A tumor (cancer) in the pancreas may grow without any symptoms at first. This means the cancer is often advanced when it is first found.
Symptoms of pancreatic cancer include:
- Diarrhea
- Dark urine and clay-colored stools
-
Fatigue
and weakness
Fatigue
Fatigue is a feeling of weariness, tiredness, or lack of energy.
Read Article Now Book Mark Article - Sudden increase in blood sugar level (diabetes)
-
Jaundice
(a yellow color in the skin, mucous membranes, or white part of the eyes) and itching of the skin
Jaundice
Jaundice is a yellow color of the skin, mucus membranes, or eyes. The yellow coloring comes from bilirubin, a byproduct of old red blood cells. Jau...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Loss of appetite and weight loss
- Nausea and vomiting
- Pain or discomfort in the upper part of the belly or abdomen
Exams and Tests
The doctor will perform a physical exam and ask about your symptoms. During the exam, the doctor may feel a lump (mass) in your abdomen.
Blood tests that may be ordered include:
-
Complete blood count (
CBC
)
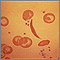
CBC
A complete blood count (CBC) test measures the following:The number of red blood cells (RBC count)The number of white blood cells (WBC count)The tota...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Liver function tests
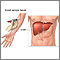
Liver function tests
Liver function tests are common tests that are used to see how well the liver is working. Tests include:AlbuminAlpha-1 antitrypsin Alkaline phosph...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Serum bilirubin
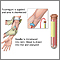
Serum bilirubin
The bilirubin blood test measures the level of bilirubin in the blood. Bilirubin is a yellowish pigment found in bile, a fluid made by the liver. Bi...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
Imaging tests that may be ordered include:
-
CT scan of the abdomen
CT scan of the abdomen
An abdominal CT scan is an imaging method. This test uses x-rays to create cross-sectional pictures of the belly area. CT stands for computed tomog...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Endoscopic retrograde cholangiopancreatography (
ERCP
)
ERCP
ERCP is short for endoscopic retrograde cholangiopancreatography. It is a procedure that looks at the bile ducts. It is done through an endoscope. ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Endoscopic
ultrasound
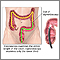
Endoscopic
Endoscopy is a way of looking inside the body using a flexible tube that has a small camera and light on the end of it. This instrument is called an...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
MRI of the abdomen
MRI of the abdomen
An abdominal magnetic resonance imaging scan is an imaging test that uses powerful magnets and radio waves. The waves create pictures of the inside ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
Diagnosis of pancreatic cancer (and what type) is made by a pancreatic biopsy .
Pancreatic biopsy
A biliary tract biopsy is the removal of small amounts of cells and fluids from the duodenum, bile ducts, pancreas, or pancreatic duct. The sample i...

If tests confirm you have pancreatic cancer, more tests will be done to see how far the cancer has spread within and outside the pancreas. This is called staging. Staging helps guide treatment and gives you an idea of what to expect.
Treatment
Treatment for adenocarcinoma depends on the stage of the tumor.
Surgery may be done if the tumor has not spread or has spread very little. Along with surgery, chemotherapy or radiation therapy or both may be used before or after surgery. A small number of people can be cured with this treatment approach.
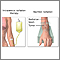
Chemotherapy
The term chemotherapy is used to describe cancer-killing drugs. Chemotherapy may be used to:Cure the cancerShrink the cancerPrevent the cancer from ...
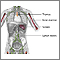
Radiation therapy
Radiation therapy uses high-powered x-rays, particles, or radioactive seeds to kill cancer cells.
When the tumor has not spread out of the pancreas but cannot be surgically removed, chemotherapy and radiation therapy together may be recommended.
When the tumor has spread (metastasized) to other organs such as the liver, chemotherapy alone is usually used.
With advanced cancer, the goal of treatment is to manage pain and other symptoms. For example, if the tube that carries bile is blocked by the pancreatic tumor, a procedure to place a tiny metal tube (stent) may be done to open the blockage. This can help relieve loss of appetite, jaundice, and itching of the skin.
Support Groups
You can ease the stress of illness by joining a cancer support group . Sharing with others who have common experiences and problems can help you not feel alone.
Cancer support group
The following organizations are good resources for information on cancer:American Cancer Society -- www. cancer. orgCancerCare -- www. cancercare. or...
Outlook (Prognosis)
Some people with pancreatic cancer that can be surgically removed are cured. But in most people, the tumor has spread and cannot be completely removed at the time of diagnosis.
Chemotherapy and radiation are often given after surgery to increase the cure rate (this is called adjuvant therapy). For pancreatic cancer that cannot be removed completely with surgery or cancer that has spread beyond the pancreas, a cure is not possible. In this case, chemotherapy is given to improve and extend one's life.
When to Contact a Medical Professional
Call for an appointment with your health care provider if you have:
- Abdominal pain that does not go away
- Back pain
- Loss of appetite
- Unexplained fatigue or weight loss
- Other symptoms of this disorder
Prevention
Preventive measures include:
- If you smoke, now is the time to quit.
- Keep a diet high in fruits, vegetables, and whole grains.
- Exercise regularly to stay at a healthy weight.
References
Mauro LA, Herman JM, Jaffee EM, Laheru DA. Carcinoma of the pancreas. In: Niederhuber JE, Armitage JO, Doroshow JH, Kastan MB, Tepper JE, eds. Abeloff's Clinical Oncology . 5th ed. Philadelphia, PA: Elsevier Churchill Livingstone; 2014:chap 81.
National Cancer Institute. PDQ Pancreatic cancer treatment. Bethesda, MD. www.cancer.gov. Date last modified July 10, 2015. http://www.cancer.gov/types/pancreatic/hp/pancreatic-treatment-pdq. Accessed October 7, 2015.
National Comprehensive Cancer Network. NCCN Clinical Practice Guidelines in Oncology: Pancreatic adenocarcinoma. Version 2.2015. http://www.nccn.org/professionals/physician_gls/pdf/pancreatic.pdf. Accessed October 7, 2015.
Shires GT, Wilfong LS. Pancreatic cancer, cystic pancreatic neoplasms, and other nonendocrine pancreatic tumors. In: Feldman M, Friedman LS, Brandt LJ, eds. Sleisenger and Fordtran's Gastrointestinal and Liver Disease: Pathophysiology/Diagnosis/Management . 10th ed. Philadelphia, PA: Elsevier Saunders; 2016:chap 60.
-
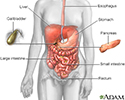
Digestive system - illustration
The esophagus, stomach, large and small intestine, aided by the liver, gallbladder and pancreas convert the nutritive components of food into energy and break down the non-nutritive components into waste to be excreted.
Digestive system
illustration
-
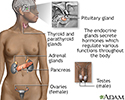
Endocrine glands - illustration
Endocrine glands release hormones (chemical messengers) into the bloodstream to be transported to various organs and tissues throughout the body. For instance, the pancreas secretes insulin, which allows the body to regulate levels of sugar in the blood. The thyroid gets instructions from the pituitary to secrete hormones which determine the pace of chemical activity in the body (the more hormone in the bloodstream, the faster the chemical activity; the less hormone, the slower the activity).
Endocrine glands
illustration
-
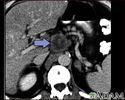
Pancreatic cancer, CT scan - illustration
A CT scan of the upper abdomen showing a tumor (pancreas carcinoma) in the head of the pancreas, seen here in the middle of the picture.
Pancreatic cancer, CT scan
illustration
-
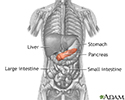
Pancreas - illustration
The pancreas is an elongated, tapered gland that is located behind the stomach and secretes digestive enzymes and the hormones insulin and glucagon.
Pancreas
illustration
-
Biliary obstruction - series
Presentation
-
Digestive system - illustration
The esophagus, stomach, large and small intestine, aided by the liver, gallbladder and pancreas convert the nutritive components of food into energy and break down the non-nutritive components into waste to be excreted.
Digestive system
illustration
-
Endocrine glands - illustration
Endocrine glands release hormones (chemical messengers) into the bloodstream to be transported to various organs and tissues throughout the body. For instance, the pancreas secretes insulin, which allows the body to regulate levels of sugar in the blood. The thyroid gets instructions from the pituitary to secrete hormones which determine the pace of chemical activity in the body (the more hormone in the bloodstream, the faster the chemical activity; the less hormone, the slower the activity).
Endocrine glands
illustration
-
Pancreatic cancer, CT scan - illustration
A CT scan of the upper abdomen showing a tumor (pancreas carcinoma) in the head of the pancreas, seen here in the middle of the picture.
Pancreatic cancer, CT scan
illustration
-
Pancreas - illustration
The pancreas is an elongated, tapered gland that is located behind the stomach and secretes digestive enzymes and the hormones insulin and glucagon.
Pancreas
illustration
-
Biliary obstruction - series
Presentation
Review Date: 8/1/2015
Reviewed By: Yi-Bin Chen, MD, Leukemia/Bone Marrow Transplant Program, Massachusetts General Hospital, Boston, MA. Also reviewed by David Zieve, MD, MHA, Isla Ogilvie, PhD, and the A.D.A.M. Editorial team.