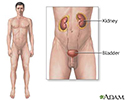
Atheroembolic renal disease
Renal disease - atheroembolic; Cholesterol embolization syndrome; Atheroemboli - renal; Atherosclerotic disease - renal
Atheroembolic renal disease (AERD) occurs when small particles made of hardened cholesterol and fat spread to the small blood vessels of the kidneys.
Causes
AERD is linked to atherosclerosis . Atherosclerosis is a common disorder of the arteries. It occurs when fat, cholesterol, and other substances build up in the walls of arteries and form a hard substance called plaque.
Atherosclerosis
Hardening of the arteries, also called atherosclerosis, occurs when fat, cholesterol, and other substances build up in the walls of arteries. These ...

In AERD, cholesterol crystals break off from the plaque lining the arteries. These crystals move into the bloodstream. Once in circulation, the crystals get stuck in tiny blood vessels called arterioles. There, they reduce blood flow to tissues and cause swelling (inflammation) and tissue damage that can harm the kidneys or other parts of the body. Acute arterial occlusion occurs when the artery that supplies blood to the kidney suddenly becomes blocked.
Acute arterial occlusion
Acute arterial occlusion of the kidney is a sudden, severe blockage of the artery that supplies blood to the kidney.
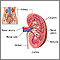
The kidneys are involved about half of the time. Other body parts that may be involved include the skin, eyes, muscles and bones, brain and nerves, and organs in the abdomen. Acute kidney failure is possible if the blockages of the kidney blood vessels are severe.
Acute kidney failure
Acute kidney failure is the rapid (less than 2 days) loss of your kidneys' ability to remove waste and help balance fluids and electrolytes in your b...

Atherosclerosis of the aorta is the most common cause of AERD. The cholesterol crystals may also break off during aortic angiography , cardiac catheterization , or surgery of the aorta or other major arteries.
Aortic angiography
Aortic angiography is a procedure that uses a special dye and x-rays to see how blood flows through the aorta. The aorta is the major artery leading...
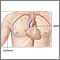
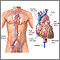
Cardiac catheterization
Cardiac catheterization involves passing a thin flexible tube (catheter) into the right or left side of the heart. The catheter is most often insert...
In some cases, AERD may occur without a known cause.
The risk factors for AERD are the same as risk factors for atherosclerosis, including age, male gender, cigarette smoking, high blood pressure, and diabetes.
References
DuBose TD Jr, Santos RM. Vascular disorders of the kidney. In: Goldman L, Schafer AI, eds. Goldman's Cecil Textbook of Medicine . 24th ed. Philadelphia, PA: Elsevier Saunders; 2011:chap 127.
Ruggenenti P, Cravedi P, Remuzzi G. Microvascular and macrovascular diseases of the kidney. In: Taal MW, Chertow GM, Marsden PA, Skorecki K, Yu A, Brenner BM, eds. Brenner and Rector's The Kidney . 9th ed. Philadelphia, PA; Elsevier Saunders; 2011:chap 34.
Review Date: 11/26/2014
Reviewed By: Charles Silberberg DO, Private Practice specializing in Nephrology, Affiliated with New York Medical College, Division of Nephrology, Valhalla, NY. Review provided by VeriMed Healthcare Network. Also reviewed by David Zieve, MD, MHA, Isla Ogilvie, PhD, and the A.D.A.M. Editorial team.