Prostatitis - nonbacterial
NBP; Prostatodynia; Pelvic pain syndrome; CPPS; Chronic nonbacterial prostatitis; Chronic genitourinary pain
Chronic nonbacterial prostatitis causes long-term pain and urinary symptoms. It involves the prostate gland or other parts of a man's lower urinary tract or genital area. This condition is not caused by an infection with bacteria .
Infection with bacteria
Prostatitis is swelling of the prostate gland. Prostate tissue becomes inflamed. This problem can be caused by an infection with bacteria. Acute pr...
Causes
Possible causes of nonbacterial prostatitis include:
- A past bacterial prostatitis infection
- Bicycle riding
- Less common types of bacteria
- Irritation caused by a backup of urine flowing into the prostate
- Irritation from chemicals
- Nerve problem involving the lower urinary tract
- Parasites
- Pelvic floor muscle problem
- Sexual abuse
- Viruses
Life stresses and emotional factors may play a part in the problem.
Most men with chronic prostatitis have the nonbacterial form.
Symptoms
Symptoms may include:
- Blood in the semen
- Blood in the urine
- Pain in the genital area and lower back
- Pain with bowel movements
- Pain with ejaculation
- Problems with urinating
Exams and Tests
Most of the time a physical exam is normal. However, the prostate may be swollen or tender.
Urine tests may show white or red blood cells in the urine. A semen culture may show a higher number of white blood cells and low sperm count with poor movement.
Urine culture or culture from the prostate does not show bacteria.
Treatment
Treatment for nonbacterial prostatitis is difficult. The problem is hard to cure, so the goal is to control symptoms.
Several types of medicines may be used to treat the condition. These include:
- Long-term antibiotics to make sure that the prostatitis is not caused by bacteria. However, people who are not helped by antibiotics should stop taking these medicines.
- Drugs called alpha-adrenergic blockers help relax the muscles of the prostate gland. It often takes about 6 weeks before these medicines start working. Many people do not get relief from these medicines.
- Aspirin, ibuprofen, and other nonsteroidal anti-inflammatory drugs (NSAIDs), which may relieve symptoms for some men.
- Muscle relaxers like diazepam or cyclobenzaprine can help to reduce spasms in the pelvic floor.
Some people have found some relief from pollen extract (Cernitin) and allopurinol, although research does not confirm their benefit. Stool softeners may help reduce discomfort with bowel movements.
Surgery, called transurethral resection of the prostate , may be done in rare cases if medicine does not help. This surgery is not done on younger men in most cases. It may cause retrograde ejaculation . This can lead to sterility, impotence , and incontinence .
Transurethral resection of the prostate
Transurethral resection of the prostate is a surgery to remove the inside part of the prostate gland. It is done in order to treat symptoms of an en...

Retrograde ejaculation
Retrograde ejaculation occurs when semen enters the bladder instead of going out through the urethra during ejaculation.

Impotence
An erection problem occurs when a man cannot get or keep an erection that is firm enough for intercourse. You may not be able to get an erection at ...

Incontinence
Urinary (or bladder) incontinence happens when you are not able to keep urine from leaking out of your urethra. The urethra is the tube that carries...
Other treatments that may be tried include:
- Warm baths to ease some of the pain.
- Prostate massage, acupuncture, and relaxation exercises. However, none of these therapies have been proven to be effective.
- Dietary changes to avoid bladder and urinary tract irritants.
Outlook (Prognosis)
Many people respond to treatment. However, others do not get relief, even after trying many things. Symptoms often come back and may not be treatable.
Possible Complications
Untreated symptoms of nonbacterial prostatitis may lead to sexual and urinary problems. These problems can affect your lifestyle and emotional well-being.
When to Contact a Medical Professional
Call your health care provider if you have symptoms of prostatitis.
References
Kaplan SA. Benign prostatic hyperplasia and prostatitis. In: Goldman L, Schafer AI, eds. Goldman's Cecil Medicine . 25th ed. Philadelphia, PA: Elsevier Saunders; 2016:chap 129.
Nickel JC. In: Wein AJ, ed. Prostatitis and related conditions, orchitis, and epididymitis. Campbell-Walsh Urology . 10th ed. Philadelphia, PA: Elsevier Saunders; 2012:chap 11.
-
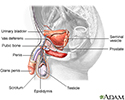
Male reproductive anatomy - illustration
The male reproductive structures include the penis, the scrotum, the seminal vesicles and the prostate.
Male reproductive anatomy
illustration
Review Date: 8/31/2015
Reviewed By: Jennifer Sobol, DO, urologist at the Michigan Institute of Urology, West Bloomfield, MI. Review provided by VeriMed Healthcare Network. Also reviewed by David Zieve, MD, MHA, Isla Ogilvie, PhD, and the A.D.A.M. Editorial team.