Brain surgery
Craniotomy; Surgery - brain; Neurosurgery; Craniectomy; Stereotactic craniotomy; Stereotactic brain biopsy; Endoscopic craniotomy
Brain surgery is an operation to treat problems in the brain and surrounding structures.
Description
Before surgery, the hair on part of the scalp is shaved and the area is cleaned. The doctor makes a surgical cut through the scalp. The location of this cut depends on where the problem in the brain is located.
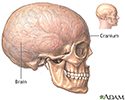
The surgeon creates a hole in the skull and removes a bone flap.
If possible, the surgeon will make a smaller hole and insert a tube with a light and camera on the end. This is called an endoscope. The surgery will be done with tools placed through the endoscope. MRI or CT scan can help guide the doctor to the proper place in the brain.
MRI
A head MRI (magnetic resonance imaging) is an imaging test that uses powerful magnets and radio waves to create pictures of the brain and surrounding...
CT
A computed tomography (CT) scan is an imaging method that uses x-rays to create pictures of cross-sections of the body. Related tests include:Abdomin...

During surgery, your surgeon may:
-
Clip off an
aneurysm
to prevent blood flow
Aneurysm
An aneurysm is a weak area in the wall of a blood vessel that causes the blood vessel to bulge or balloon out. When an aneurysm occurs in a blood ve...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Remove a
tumor
or a piece of tumor for a
biopsy
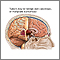
Tumor
A primary brain tumor is a group (mass) of abnormal cells that start in the brain.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark ArticleBiopsy
A biopsy is the removal of a small piece of tissue for laboratory examination.
Read Article Now Book Mark Article - Remove abnormal brain tissue
- Drain blood or an infection
- Free a nerve
The bone flap is usually replaced after surgery, using small metal plates, sutures, or wires. The bone flap may not be put back if your surgery involved a tumor or an infection, or if the brain was swollen. (This is called a craniectomy.)
The time it takes for the surgery depends on the problem being treated.
Why the Procedure Is Performed
Brain surgery may be done if you have:
- Brain tumor
- Bleeding (hemorrhage) in the brain
-
Blood clots
(
hematomas
) in the brain
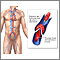
Blood clots
Blood clots are clumps that occur when blood hardens from a liquid to a solid. A blood clot that forms inside one of your veins or arteries is calle...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark ArticleHematomas
Bleeding into the skin can occur from broken blood vessels that form tiny red dots (called petechiae). Blood also can collect under the tissue in la...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Weaknesses in blood vessels (
brain aneurysm repair
)
Brain aneurysm repair
Brain aneurysm repair is surgery to correct an aneurysm. This is a weak area in a blood vessel wall that causes the vessel to bulge or balloon out a...
Read Article Now Book Mark Article - Abnormal blood vessels in the brain (arteriovenous malformations; AVM)
- Damage to tissues covering the brain (dura)
-
Infections in the brain (
brain abscesses
)
Brain abscesses
A brain abscess is a collection of pus, immune cells, and other material in the brain, usually from a bacterial or fungal infection.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Severe nerve or face pain (such as
trigeminal neuralgia
or
tic douloureux
)
Trigeminal neuralgia
Trigeminal neuralgia (TN) is a nerve disorder. It causes a stabbing or electric shock-like pain in parts of the face.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark ArticleTic douloureux
Trigeminal neuralgia (TN) is a nerve disorder. It causes a stabbing or electric shock-like pain in parts of the face.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Skull fracture
- Pressure in the brain after an injury or stroke
-
Epilepsy
Epilepsy
Epilepsy is a brain disorder in which a person has repeated seizures over time. Seizures are episodes of uncontrolled and abnormal firing of brain c...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Certain brain diseases (such as Parkinson disease) that may be helped with an implanted electronic device
-
Hydrocephalus
Hydrocephalus
Hydrocephalus is a buildup of fluid inside the skull that leads to brain swelling. Hydrocephalus means "water on the brain. "
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
Risks
Risks for anesthesia and surgery in general are:
- Reactions to medications, problems breathing
- Bleeding, blood clots, infection
Possible risks of brain surgery are:
- Problems with speech, memory, muscle weakness , balance, vision, coordination, and other functions. These problems may last a short while or they may not go away.
- Blood clot or bleeding in the brain
- Seizures
- Stroke
- Coma
- Infection in the brain, wound, or skull
- Brain swelling
Before the Procedure
Your doctor will examine you, and may order laboratory and imaging tests.
Tell your doctor or nurse:
- If you could be pregnant
- What drugs you are taking, even drugs, supplements, vitamins, or herbs you bought without a prescription
- If you have been drinking a lot of alcohol
- If you take aspirin or anti-inflammatory drugs such as ibuprofen
- If you have allergies or reactions to medications or iodine
During the days before the surgery:
- You may be asked to stop taking aspirin, ibuprofen, warfarin (Coumadin), and any other medicines that make it hard for your blood to clot.
- Ask your doctor which drugs you should still take on the day of the surgery.
- Try to stop smoking. Smoking can slow healing after your operation. Ask your doctor for help.
- Your doctor or nurse may ask you to wash your hair with a special shampoo the night before surgery.
On the day of the surgery:
- You will likely be asked not to drink or eat anything for 8 to 12 hours before the surgery.
- Take the drugs your doctor told you to take with a small sip of water.
- Arrive at the hospital on time.
After the Procedure
After surgery, you will be closely monitored by your health care team to make sure your brain is working properly. The doctor or nurse may ask you questions, shine a light in your eyes, and ask you to do simple tasks. You may need oxygen for a few days.
The head of your bed will be kept raised to help reduce swelling of your face or head. The swelling is normal after surgery.
Medicines will be given to relieve pain.
You will usually stay in the hospital for 3 to 7 days. You may need physical therapy (rehabilitation).
After you go home, follow any self-care instructions you're given.
Self-care instructions
You had surgery on your brain. During surgery, your doctor made a surgical cut (incision) in your scalp. A small hole was then drilled into your sk...
Outlook (Prognosis)
How well you do after brain surgery depends on the condition being treated, your general health, which part of the brain is involved, and the specific type of surgery.
References
Gasco J, Mohanty A, Hanbali F, Patterson JT. Neurosurgey. In: Townsend CM, Beauchamp RD, Evers BM, Mattox KL, eds. Sabiston Textbook of Surgery . 19th ed. Philadelphia, PA: Elsevier Saunders; 2012:chap 68.
-
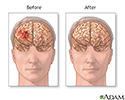
Before and after hematoma repair - illustration
Brain surgery may be needed in treatment of subdural hematoma to remove blood and to decrease intracranial pressure. The outcome of the surgery depends on the source, severity, and location of the problem.
Before and after hematoma repair
illustration
-
Craniotomy - series
Presentation
-
Before and after hematoma repair - illustration
Brain surgery may be needed in treatment of subdural hematoma to remove blood and to decrease intracranial pressure. The outcome of the surgery depends on the source, severity, and location of the problem.
Before and after hematoma repair
illustration
-
Craniotomy - series
Presentation
Review Date: 2/3/2015
Reviewed By: Amit M. Shelat, DO, FACP, Attending Neurologist and Assistant Professor of Clinical Neurology, SUNY Stony Brook, School of Medicine, Stony Brook, NY. Review provided by VeriMed Healthcare Network. Also reviewed by David Zieve, MD, MHA, Isla Ogilvie, PhD, and the A.D.A.M. Editorial team.