Vision - night blindness
Nyctanopia; Nyctalopia; Night blindness
Night blindness is poor vision at night or in dim light.
Considerations
Night blindness may cause problems with driving at night. People with night blindness often have trouble seeing stars on a clear night or walking through a dark room, such as a movie theater.
These problems are often worse just after a person is in a brightly lit environment. Milder cases may just have a harder time adapting to darkness.
Causes
The causes of night blindness fall into 2 categories: treatable and nontreatable.
Treatable causes:
- Cataracts
-
Nearsightedness
Nearsightedness
Nearsightedness is when light entering the eye is focused incorrectly. This makes distant objects appear blurred. Nearsightedness is a type of refr...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Use of certain drugs
-
Vitamin A deficiency
(rare)
Vitamin A deficiency
Vitamin A is a fat-soluble vitamin that is stored in the liver. There are two types of vitamin A that are found in the diet. Preformed vitamin A is...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
Nontreatable causes:
- Birth defects
-
Retinitis pigmentosa
Retinitis pigmentosa
Retinitis pigmentosa is an eye disease in which there is damage to the retina. The retina is the layer of tissue at the back of the inner eye. This...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
Home Care
Take safety measures to prevent accidents in areas of low light. Avoid driving a car at night, unless you get your eye doctor's approval.
Vitamin A supplements may be helpful if you have a vitamin A deficiency. Ask your health care provider.
When to Contact a Medical Professional
It is important to have a complete eye exam to determine the cause, which may be treatable. Call your eye doctor if symptoms of night blindness persist or significantly affect your life.
What to Expect at Your Office Visit
Your provider will examine you and your eyes. The goal of the medical exam is to determine if the problem can be corrected (for example, with new glasses or cataract removal ), or if the problem is due to something that is not treatable.
Cataract removal
Cataract removal is surgery to remove a clouded lens (cataract) from the eye. Cataracts are removed to help you see better. The procedure almost al...

The provider may ask you questions, including:
- How severe is the night blindness?
- When did your symptoms start?
- Did it occur suddenly or gradually?
- Does it happen all the time?
- Does using corrective lenses improve night vision?
- Have you ever had eye surgery?
- What medicines do you use?
- How is your diet?
- Have you recently injured your eyes or head?
-
Do you have a family history of
diabetes
?
Diabetes
Diabetes is a chronic disease in which the body cannot regulate the amount of sugar in the blood.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Do you have other vision changes?
- What other symptoms do you have?
- Do you have unusual stress, anxiety, or a fear of the dark?
The eye exam will include:
- Color vision testing
- Pupil light reflex
- Refraction
- Retinal exam
-
Slit lamp examination
Slit lamp examination
The slit-lamp examination looks at structures that are at the front of the eye.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Visual acuity
Other tests may be done:
-
Electroretinogram
(ERG)
Electroretinogram
Electroretinography is a test to measure the electrical response of the eye's light-sensitive cells, called rods and cones. These cells are part of ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Visual field
Visual field
The visual field refers to the total area in which objects can be seen in the side (peripheral) vision as you focus your eyes on a central point. Thi...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
References
Cukras CA, Zein WM, Caruso RC, Sieving PA. Progressive and ‘stationary’ inherited retinal degenerations. In: Yanoff M, Duker JS, eds. Ophthalmology . 4th ed. Philadelphia, PA: Elsevier Saunders; 2014:chap 6.13.
Thurtell MJ, Tomsak RL. Visual loss. In: Daroff RB, Jankovic J, Mazziotta JC, Pomeroy SL, eds. Bradley's Neurology in Clinical Practice . 7th ed. Philadelphia, PA: Elsevier Saunders; 2016:chap 16.
Tsang SH, Gouras P. Molecular physiology and pathology of the retina. In: Tansman W, Jaeger EA, eds. Duane's Ophthalmology 2013 edition . Philadelphia, PA: Lippincott Williams & Wilkins; 2013:vol 3, chap 2.
-
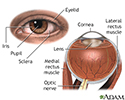
External and internal eye anatomy - illustration
The cornea allows light to enter the eye. As light passes through the eye the iris changes shape by expanding and letting more light through or constricting and letting less light through to change pupil size. The lens then changes shape to allow the accurate focusing of light on the retina. Light excites photoreceptors that eventually, through a chemical process, transmit nerve signals through the optic nerve to the brain. The brain processes these nerve impulses into sight.
External and internal eye anatomy
illustration
-
External and internal eye anatomy - illustration
The cornea allows light to enter the eye. As light passes through the eye the iris changes shape by expanding and letting more light through or constricting and letting less light through to change pupil size. The lens then changes shape to allow the accurate focusing of light on the retina. Light excites photoreceptors that eventually, through a chemical process, transmit nerve signals through the optic nerve to the brain. The brain processes these nerve impulses into sight.
External and internal eye anatomy
illustration
Review Date: 8/20/2016
Reviewed By: Franklin W. Lusby, MD, ophthalmologist, Lusby Vision Institute, La Jolla, CA. Also reviewed by David Zieve, MD, MHA, Isla Ogilvie, PhD, and the A.D.A.M. Editorial team.