Heart murmurs
Chest sounds - murmurs; Heart sounds - abnormal; Murmur - innocent; Innocent murmur; Systolic heart murmur; Diastolic heart murmur
A heart murmur is a blowing, whooshing, or rasping sound heard during a heartbeat. The sound is caused by turbulent (rough) blood flow through the heart valves or near the heart.
Considerations
The heart has 4 chambers:
- Two upper chambers (atria)
- Two lower chambers (ventricles)
The heart has valves that close with each heartbeat, causing blood to flow in only one direction. The valves are located between the chambers.
Murmurs can happen for many reasons, such as:
- When a valve does not close tightly and blood leaks backward (regurgitation)
- When blood flows through a narrowed or stiff heart valve (stenosis)
There are several ways in which your health care provider may describe a murmur:
- Murmurs are classified ("graded") depending on how loud the murmur sounds with a stethoscope. The grading is on a scale. Grade I can barely be heard. An example of a murmur description is a "grade II/VI murmur." (This means the murmur is grade 2 on a scale of 1 to 6).
- In addition, a murmur is described by the stage of the heartbeat when the murmur is heard. A heart murmur may be described as systolic or diastolic.
When a murmur is more noticeable, the provider may be able to feel it with the palm of the hand over the heart.
Things the provider will look for in the exam include:
- Does the murmur occur when the heart is resting or contracting?
- Does it last throughout the heartbeat?
- Does it change when you move?
- Can it be heard in other parts of the chest, on the back, or in the neck?
- Where is the murmur heard the loudest?
Causes
Many heart murmurs are harmless. These types of murmurs are called innocent murmurs. They will not cause any symptoms or problems. Innocent murmurs DO NOT need treatment.
Other heart murmurs may indicate an abnormality in the heart. These abnormal murmurs can be caused by:
-
Problems of the aortic valve (
aortic regurgitation
, aortic stenosis)
Aortic regurgitation
Aortic insufficiency is a heart valve disease in which the aortic valve does not close tightly. This allows blood to flow from the aorta (the larges...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Problems of the mitral valve (
chronic
or acute mitral regurgitation,
mitral stenosis
)
Chronic
Mitral regurgitation is a disorder in which the mitral valve on the left side of the heart does not close properly. Regurgitation means leaking from ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark ArticleMitral stenosis
Mitral stenosis is a disorder in which the mitral valve does not fully open. This restricts the flow of blood.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Hypertrophic cardiomyopathy
(idiopathic hypertrophic subaortic stenosis)
Hypertrophic cardiomyopathy
Hypertrophic cardiomyopathy (HCM) is a condition in which the heart muscle becomes thick. Often, only 1 part of the heart is thicker than the other ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article - Pulmonary regurgitation (backflow of blood into the right ventricle, caused by failure of the pulmonary valve to close completely)
-
Pulmonary valve stenosis
Pulmonary valve stenosis
Pulmonary valve stenosis is a heart valve disorder that involves the pulmonary valve. This is the valve separating the right ventricle (one of the ch...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Problems of the tricuspid valve (
tricuspid regurgitation
, tricuspid stenosis)
Tricuspid regurgitation
Blood that flows between different chambers of your heart must pass through a heart valve. These valves open up enough so that blood can flow throug...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
Significant murmurs in children are more likely to be caused by:
- Anomalous pulmonary venous return (an abnormal formation of the pulmonary veins)
-
Atrial septal defect
(ASD)
Atrial septal defect
Atrial septal defect (ASD) is a heart defect that is present at birth (congenital). As a baby develops in the womb, a wall (septum) forms that divide...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Coarctation of the aorta
Coarctation of the aorta
The aorta carries blood from the heart to the vessels that supply the body with blood. If part of the aorta is narrowed, it is hard for blood to pas...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Patent ductus arteriosus
(PDA)
Patent ductus arteriosus
Patent ductus arteriosus (PDA) is a condition in which the ductus arteriosus does not close. The word "patent" means open. The ductus arteriosus is ...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Ventricular septal defect
(VSD)
Ventricular septal defect
Ventricular septal defect is a hole in the wall that separates the right and left ventricles of the heart. Ventricular septal defect is one of the m...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
Multiple murmurs may result from a combination of heart problems.
Children often have murmurs as a normal part of development. These murmurs DO NOT need treatment. They may include:
- Pulmonary flow murmurs
- Still's murmur
- Venous hum
What to Expect at Your Office Visit
A provider can listen to your heart sounds by placing a stethoscope over your chest. You will be asked questions about your medical history and symptoms, such as:
- Have other family members had murmurs or other abnormal heart sounds?
- Do you have a family history of heart problems?
- Do you have chest pain, fainting, shortness of breath, or other breathing problems?
- Have you had swelling, weight gain, or bulging veins in the neck?
- Does your skin have a bluish color?
The provider may ask you to squat, stand, or hold your breath while bearing down or gripping something with your hands to listen to your heart.
The following tests may be done:
-
Chest x-ray
Chest x-ray
A chest x-ray is an x-ray of the chest, lungs, heart, large arteries, ribs, and diaphragm.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
ECG
ECG
An electrocardiogram (ECG) is a test that records the electrical activity of the heart.
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article -
Echocardiography
Echocardiography
An echocardiogram is a test that uses sound waves to create pictures of the heart. The picture and information it produces is more detailed than a s...
 ImageRead Article Now Book Mark Article
ImageRead Article Now Book Mark Article
References
Fang JC, O'Gara PT. The history and physical examination: An evidence-based approach. In: Bonow RO, Mann DL, Zipes DP, Libby P, Braunwald E, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine . 10th ed. Philadelphia, PA: Elsevier Saunders; 2015:chap 11.
Goldman L. Approach to the patient with possible cardiovascular disease. In: Goldman L, Schafer AI, eds. Goldman's Cecil Medicine . 25th ed. Philadelphia, PA: Elsevier Saunders; 2016:chap 51.
Nishimura RA, Otto CM, Bonow RO, et al. 2014 AHA/ACC guideline for the management of patients with valvular heart disease: executive summary: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. Circulation . 2014;129(23):2440-2492. PMID: 24589852 www.ncbi.nlm.nih.gov/pubmed/24589852 .
-
Heartbeat
Animation
-
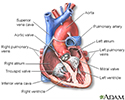
Heart, section through the middle - illustration
The interior of the heart is composed of valves, chambers, and associated vessels.
Heart, section through the middle
illustration
-
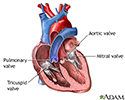
Heart valves - illustration
The valves of the heart open and close to control the flow of blood entering or leaving the heart.
Heart valves
illustration
-
Heart, section through the middle - illustration
The interior of the heart is composed of valves, chambers, and associated vessels.
Heart, section through the middle
illustration
-
Heart valves - illustration
The valves of the heart open and close to control the flow of blood entering or leaving the heart.
Heart valves
illustration
Review Date: 5/5/2016
Reviewed By: Michael A. Chen, MD, PhD, Associate Professor of Medicine, Division of Cardiology, Harborview Medical Center, University of Washington Medical School, Seattle, WA. Also reviewed by David Zieve, MD, MHA, Isla Ogilvie, PhD, and the A.D.A.M. Editorial team.